Twin-to-twin Transfusion Syndrome – Stages, Causes, and Symptoms
TTTS (twin-to-twin transfusion syndrome) is an uncommon and dangerous illness that can develop during pregnancy. When identical twins share a placenta, the TTTS occurs (monochorionic). Abnormal blood vessels connections happen in the placenta. They allow for unequal blood flow between the fetuses – one of the twins, referred to as the donor, gets dehydrated, while the receiver, the other twin, gets excessive blood pressure. The recipient excretes an excessive amount of urine, overfilling the amniotic sac.
What Is Twin-to-twin Transfusion Syndrome (TTTS)?
The twin-to-twin transfusion syndrome (TTTS) is a disorder in which the fetuses share a placenta but are in two different amniotic sacs (monochorionic-diamniotic or “mono-di”). How common is twin to twin transfusion syndrome? It occurs in 10-15% of identical twin pregnancies. The placenta ordinarily maintains intricate blood flow networks that regulate blood flow via each fetus’ umbilical cord.
In TTTS, however, these networks have aberrant connections, disrupting the usual balance and resulting in low blood flow to one twin (donor) and excessive blood flow to the other (recipient). As a result, the donor twin suffers from low blood pressure, slow growth, and low amniotic fluid levels (oligohydramnios). On the other hand, the receiver twin develops normally, but the increased blood supply generates high blood pressure, which causes heart strain and high amounts of amniotic fluid (polyhydramnios).
If left untreated, TTTS can cause severe prematurity and substantial damage to the heart, brain, kidneys, and other organs in either twin. It can be lethal for one or both twins in the worst-case scenario.
Stages of Twin-to-twin Transfusion Syndrome
TTTS diagnosis is a staging method utilized to classify the condition’s severity. This technique, known as the Quintero staging system, aids in determining if an intervention is required and which treatment option(s) are most suited. Here is an explanation of the stages of twin to twin transfusion syndrome:
1. Stage 1
In the twin-to-twin transfusion syndrome stage 1, the ultrasound indicates an amniotic fluid imbalance surrounding the twins, but the donor twin’s bladder is still visible. The presence of the bladder suggests that the donor baby is receiving enough nutrients and fluid from the blood to make pee.
2. Stage 2
The 2nd stage is when the ultrasound reveals an amniotic fluid imbalance around the twins, but the donor twin’s bladder is not evident. This discovery suggests that the bladder is empty, indicating that the infant has finished producing pee.
3. Stage 3
In addition to the symptoms of Stages 1 and 2, in the twin to twin transfusion syndrome stage 3, the ultrasound reveals substantial irregularities in the flow of blood within the twins’ umbilical cords.
4. Stage 4
In addition to the symptoms of Stages I-III, the recipient twin exhibits evidence of cardiac failure (hydrops fetalis or extra fluid within the baby).
Causes of Twin-to-twin Transfusion Syndrome
During pregnancy, the placenta is an extremely busy organ that gives oxygen and nourishment to the baby. It develops alongside the newborns. Sometimes, the normal flow of blood in the placenta’s arteries adopts an aberrant pattern for unknown reasons. When two pregnant infants share a placenta, blood circulation can become imbalanced, with one baby receiving too much blood through the umbilical cord and the other receiving too little. This imbalance is what causes TTTS.
Symptoms of Twin-to-twin Transfusion Syndrome
Twins experiencing TTTS exhibit varying symptoms depending on whether they are donors or receivers:
1. Donor
Donor TTTS twins receive less placental blood and lose blood to the other twin. Donor twins are smaller than donor twins both before and after birth. They are pale and anemic, have lower fetal pee flow, and have smaller bladders than typical. If the twins have two amniotic sacs, the donor twin will have less amniotic fluid than the other twin (oligohydramnios).
2. Recipient
Recipient twins get an abnormally large amount of blood from the placenta and the other twin. These infants are bigger and have an abundance of amniotic fluid (polyhydramnios). Because these infants have so much blood in their bodies, their circulatory systems may become overburdened, resulting in cardiac difficulties.
Long-term Effects of Twin-to-twin Transfusion Syndrome
Twin-twin transfusion syndrome frequently results in preterm delivery. To avoid the risk factors of TTTS, Babies in this situation require care in a neonatal critical care unit.
The vast majority of newborns who are successfully treated for twin-twin transfusion syndrome go on to enjoy normal, healthy lives. Some people, however, encounter minor problems, such as anemia. This is a simple problem to solve. Brain damage and heart failure are more significant issues. If local experts are unavailable, Cincinnati Children’s specialists can assist by providing long-term, professional care for these children.
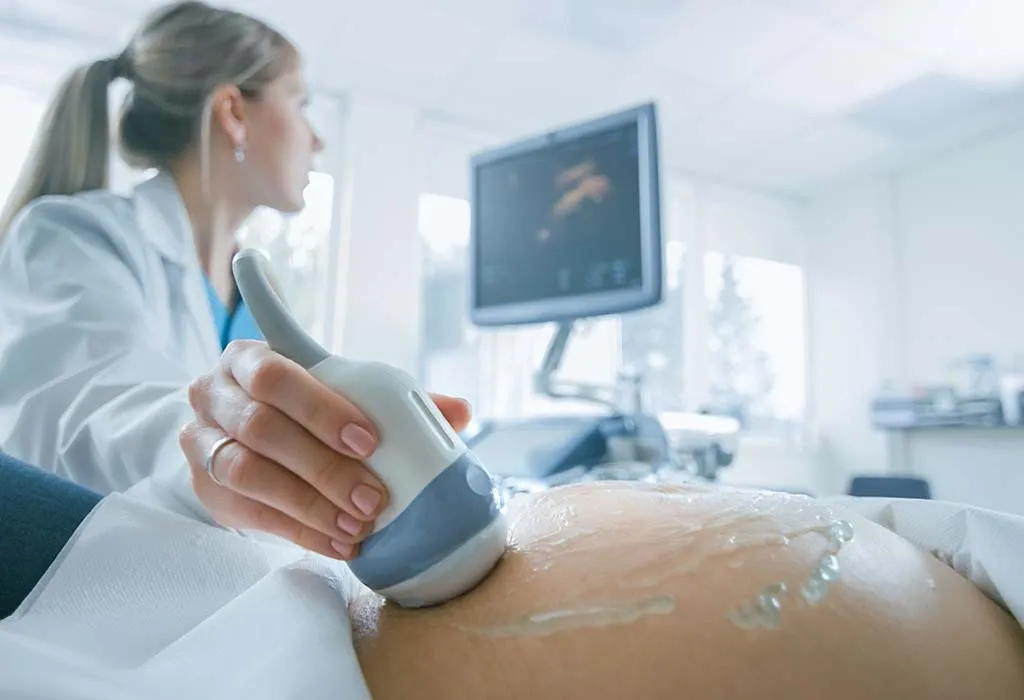
How Is Twin-to-twin Transfusion Syndrome Diagnosed?
Ultrasound confirms the diagnosis of twin to twin transfusion syndrome. When ultrasound pictures demonstrate that one child has an excess amniotic fluid and the other has much less, the problem is obvious. Blood-flow abnormalities in the umbilical cord may also be discovered. Furthermore, the mother’s uterus may grow more quickly than usual during pregnancy.
Because TTTS can progress quickly, women bearing twins who share a placenta should have regular ultrasounds to assess amniotic fluid quantities. Ultrasounds are typically conducted every two weeks, beginning at 16 weeks. During the third trimester, the frequency of ultrasounds rises.
How to Manage Twin-to-twin Transfusion Syndrome When Pregnant?
A maternal-fetal medicine specialist should monitor TTTS to identify if the stage is advancing. Progression may happen quickly, in a few days. To prevent twin to twin transfusion, some alternatives are:
1. Amnioreduction
This treatment drains extra fluid from the bigger twin, lowering amniotic pressure and lowering the risk of premature labor. Typically, fetoscopic laser photocoagulation is used.
2. Photocoagulation Using a Fetoscopic Laser
At roughly 16-26 weeks of gestation, surgeons utilize a laser to block the blood arteries that communicate between the two babies in cases with TTTS Stage 2 or higher. The surgeon inserts a pencil-tip-sized fiber-optic scope into the mother’s uterus and scans the whole placenta to detect the crossing blood vessels. Once all of these are mapped, a small laser fiber is implanted, and laser energy is used to block blood flow between the twins. Separating the blood flow of the twins is analogous to functionally separating the placenta, enabling each twin to grow independently.
3. Ultrasound Observation Using Frequent Ultrasounds
Although stage 1 instances may not necessitate intervention, it is critical to regularly monitor the twins’ growth to rule out advancement to stage 2 or beyond.
Treatment of Twin-to-twin Transfusion Syndrome
The stage of illness determines the appropriate treatment for TTTS. In most cases of TTTS (stages 1-4) that arise before 28 weeks, we advocate laser surgery since it tackles the underlying source of the disease – aberrant placental connections. If heart strain has not yet formed or the TTTS has evolved slowly after 26 weeks, a trial of observation with follow-up ultrasounds may be possible in the earliest stage I patients.
A fetal echocardiogram, sometimes known as a “fetal echo,” is a specialist ultrasound of the fetal heart that assesses cardiac strain. The fetal echo allows us to predict which individuals with stage 1 TTTS are likely to proceed to advanced stages of the illness during an observation period. Observation is not advised in these situations.
TTTS Treatment Before Birth
The key to treating twin to twin transfusion syndrome is early detection and management. The optimum treatment choice for your infants will be determined by the stage of the TTTS and the gestational age of your babies at the time of diagnosis. There are several possibilities available, including the following:
- Amnioreduction: This is a technique that is performed to reduce extra fluid from the recipient twin’s amniotic sac. The operation is similar to amniocentesis in that the clinician guides a long, extremely tiny needle into the uterus to retrieve the fluid using “real-time” ultrasound pictures. This method may be recommended for Stage 1 TTTS or when TTTS is discovered later in pregnancy when fetoscopic laser photocoagulation (see below) is no longer a possibility.
- Expectant Management: This entails close ultrasonography monitoring throughout the pregnancy. For most Stage 1 TTTS, we now prescribe expectant management.
- Fetoscopic Laser Photocoagulation: A laser is used in this minimally invasive surgery to ablate (close) blood vessels that contribute to the infants’ aberrant blood flow (Figures 3-5). Many studies have shown that this treatment for twin-to-twin transfusion syndrome is the most beneficial for newborns with advanced TTTS.
- Delivery: If TTTS is detected later in the pregnancy, having the infants delivered may be the best decision.
TTTS Treatment After Birth
If severe TTTS starts or worsens after 26 weeks of gestation, it is typically better to deliver early when the infants can survive outside the womb. The condition is automatically ended after they are born (since the twins are no longer attached). However, the consequences of the disease may not subside immediately. In most cases, they are best treated in the neonatal critical care unit shortly after delivery.
Even if the condition heals on its own (as it does in roughly 60% of early-stage TTTS patients) or if laser surgery is performed, most physicians still prefer to deliver the babies a few weeks before full term (at 36 to 37 weeks) to minimize future difficulties. Even after endoscopic laser surgery, a Cesarean section is not required unless obstetrical complications are prevalent in twin pregnancy.
TTTS is an uncommon condition that, when appropriately handled, leads to a successful pregnancy for most patients. Because of the illness’s low prevalence and peculiar physiology, most pregnant parents are ignorant of disease progression and prognosis. Now that you know more about it, stay vigilant and cooperate with your doctor to treat the condition properly.
Also Read:
Parasitic Twins
Fraternal Twins Facts
Vanishing Twin Syndrome
Was This Article Helpful?
Parenting is a huge responsibility, for you as a caregiver, but also for us as a parenting content platform. We understand that and take our responsibility of creating credible content seriously. FirstCry Parenting articles are written and published only after extensive research using factually sound references to deliver quality content that is accurate, validated by experts, and completely reliable. To understand how we go about creating content that is credible, read our editorial policy here.