Uterine Inversion – All You Need To Know

- What Is Uterine Inversion?
- How Common Uterine Inversion Is
- Grades of Inversion
- Causes of Uterine Inversion
- Symptoms of Uterine Inversion
- Diagnosis of Uterine Inversion
- Factors That Can Increase the Risk of Uterine Inversion
- Treatment for Uterine Inversion
- Will You Suffer From Uterine Inversion In Your Next Pregnancy?
- Things to Remember
Uterine inversion is a potentially fatal maternal condition where the uterus either partially or completely falls outside the cervix or even the vagina. In simple terms, it can be called “Uterus turning inside out”. In this post, we have tried to share some essential information every woman should have about the condition. Read on to know more.
What Is Uterine Inversion?
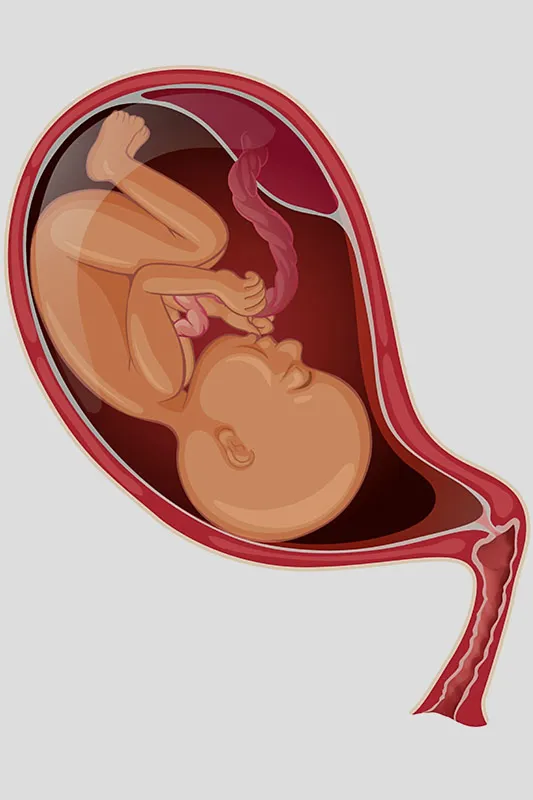
Uterine inversion is a life-threatening obstetric emergency that is very rare but can lead to serious ill effects like hypovolemic shock, severe haemorrhage, and even death in extreme conditions. The fundus of the uterus is found to pass out of the cervix and even the vagina causing an inversion of the uterus.
How Common Uterine Inversion Is
The Incidence of uterine inversion usually varies and can range from 1 case in 2000 to 1 case in every 50,000 births. In a much broader range, it can occur in about 1 in 3,000 births. The mother’s survival rate is only about 85% and can lead to death.
Based on its, severity, uterine inversion is categorised in four grades. Let’s take a look at them.
Grades of Inversion
Uterine inversion has 4 degrees or grades based on its severity.
- 1st – Incomplete inversion: The top of the uterus (fundus) has collapsed and is still inside the cavity, but if it comes out it does only till the cervix and does not exceed cervical external.
- 2nd – Complete inversion: The uterus protrudes inside-out and comes out through the cervix.
- 3rd – Prolapsed inversion: The fundus of the uterus comes out of the vagina.
- 4th – Total inversion: Both the uterine fundus and the vagina protrude inside-out beyond vaginal introitus (this is mainly seen in cases of cancer rather than childbirth).
Causes of Uterine Inversion
Major etiological factors leading to uterine inversion include:
- Excessive cord traction in the third stage of labour
- Improper discharge of placenta after childbirth
- Forceful expulsion of the placenta by doctors using medical aid
- Tension on the umbilical cord
- Prior deliveries
- Long labour (more than 24 hours)
- Use of the muscle relaxants (like magnesium sulphate) during labour
- Short umbilical cord
- Fetal macrosomia
- Excessive fundal pressure due to fundal implantation of the placenta
- Placenta accrete – Invasion of placenta deeply into the uterine walls
- Ligament laxity
- Congenital abnormalities of the uterus
Symptoms of Uterine Inversion
Some of the possible symptoms that can be noticed during uterine inversion are:
- Protrusion of uterus from the vagina
- Displacement of the uterus from its original place
- Excess loss of blood, i.e. severe haemorrhage or a rapid fall in blood pressure
- Symptoms of hypovolemic shock (lightheadedness, dizziness, coldness, tiredness, shortness of breath)
- Tachycardia – Rapid increase in heart rate
Diagnosis of Uterine Inversion
A quick and reliable diagnosis is important and can prevent maternal death. Signs of uterine inversion are as follows:
- Protrusion of vagina
- Displaced fundus from its place (abdominal area) during abdominal palpitation
- Severe haemorrhage
- Rapid fall in blood pressure (hypotension)
- Signs of shock (blood loss)
- Scans (such as ultrasound or MRI) that may be used in some cases to confirm the diagnosis
- Uterine fundus beyond vaginal introitus
- 3rd-degree inversion of the uterus
- The Echogenicity of the endometrium shows the shape of the letter C, and the echogenicity of the uterus shows the shape of the letter H during an ultrasound.
 Factors That Can Increase the Risk of Uterine Inversion
Factors That Can Increase the Risk of Uterine Inversion
Risk factors that can worsen a maternal condition that is noticed in uterine inversion include:
- Severe bleeding
- Shock
- Trauma
Treatment for Uterine Inversion
Uterine inversion management options include:
- Reposition of maternal fundus back through the cervix.
- Relaxation of the uterus using relaxants that can further help in repositioning the uterus.
- After complete placement of uterus, continuous intravenous infusion of oxytocin is provided to make the uterus firm and keep it in position, which further controls the bleeding.
- Until uterus is at its place, the doctor may keep applying pressure by using one hand inside the vagina and other over the abdominal area (superficially) to compress the uterus and stop the bleeding.
The major surgical techniques for uterine inversion management are described below:
- Huntington – Clamps are placed on the round ligament, near its insertion in the uterus, and traction is applied while the doctor exerts traction on the contralateral way through the vagina. It is the simplest technique and has a lower risk of complications.
- Haultaim – Preferred when the first technique is a failure. Here in this method, an incision is made in the posterior portion of the ring formed by the cervix in order to increase the size of the ring and thus reposition the uterus.
- Another surgical technique was given by Spinelli. In this method, the surgeon performs a dissection of the vesicouterine space and makes an incision on the cervix, allowing the uterus to return to its original position.
- Hydrostatic pressure technique is an alternative method where balloons are generally placed intravaginally and filled by a saline solution to increase the pressure on the uterine fundus resulting in pushing the uterus to its initial position.
- In extreme conditions where there are higher chances of maternal death, the uterus is completely removed by surgery.
- Monitoring of vaginal bleeding and for other symptoms will be done continuously.
- Blood transfusion is made for a proper replacement, also supplemented by antibiotics to prevent further complications like infection.
- Until the condition is stabilised, the mother is kept under close observation for any other signs of degradation in her condition.
- Post-discharge dietary changes and lifestyle modification plays an essential role; it can also be called a part of the treatment.

Will You Suffer From Uterine Inversion In Your Next Pregnancy?
Yes, there are higher chances of uterine inversion in the next pregnancy if you have already suffered one. As with any pregnancy complication or other medical problem, the complete medical history has to be provided to the doctor for proper care and management. This will help the practitioner in further reducing the complications associated with the condition.
Things to Remember
It is always advisable to keep track of medical history and provide the same to the doctor when seeking medical advice to prevent further risk of uterine inversion in the future.

Uterine inversion is a fatal condition which requires diagnosis in advance and also proper management as quickly as it occurs. Irrespective of the approach, vaginal or surgical, prompt treatment is the best way to deal with uterine inversion to prevent maternal death.
Was This Article Helpful?
Parenting is a huge responsibility, for you as a caregiver, but also for us as a parenting content platform. We understand that and take our responsibility of creating credible content seriously. FirstCry Parenting articles are written and published only after extensive research using factually sound references to deliver quality content that is accurate, validated by experts, and completely reliable. To understand how we go about creating content that is credible, read our editorial policy here.