Vasa Previa – Causes, Signs, and Treatment
- What Is Vasa Previa in Pregnancy?
- What Are the Causes of Vasa Previa?
- Symptoms of Vasa Previa
- How Is Vasa Previa Diagnosed?
- Complications Associated With Vasa Previa
- Vasa Previa Treatment
- How to Manage Vasa Previa
- Prognosis and Outcome
- What Is the Survival Rate of Babies with Vasa Previa?
Pregnancy is a time of excitement and nervousness. Anything can happen during pregnancy and that is why it is necessary to be extremely cautious in pregnancy. There are some serious conditions that mothers-to-be need to be aware of to ensure that they have a safe pregnancy and a healthy baby. One such condition is called ‘vasa previa’. It is an uncommon but serious condition that can endanger the life of the baby and cause pregnancy complications in the mother. This article tells you all you need to know about vasa previa.
What Is Vasa Previa in Pregnancy?
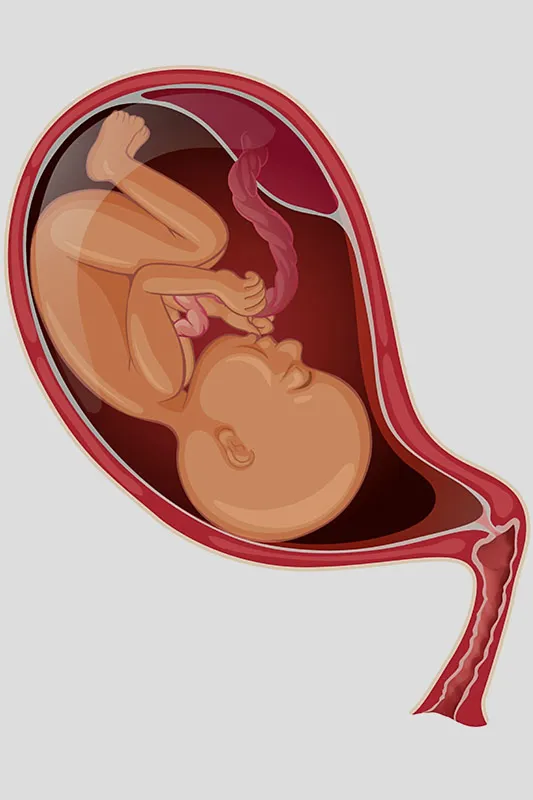
Vasa Previa is a dangerous and rare condition where the blood vessels of the foetus run across the inner cervical opening that separates the uterus from the vagina. Umbilical cord blood vessels run through the chorionic membrane and not directly into the placenta; vasa previa causes them to be unprotected by placental tissue or the umbilical cord. This makes them highly vulnerable to rupture, which causes foetal haemorrhaging. It has a high fatality rate.
What Are the Causes of Vasa Previa?
Following are the reasons that may lead to the development of this condition in pregnant women:
- Multiple Pregnancies: Moms-to-be who are carrying multiples such as twin and triplets are at a higher risk of developing vasa previa.
- IVF: Moms who became pregnant via in vitro fertilisation have an increased risk of developing vasa previa. The occurrence of ‘Vasa Previa’ in women who have conceived through IVF is as high as 1 in 300 women.
- Accessory Placental Lobes: This is a condition where the placenta does not form properly and has one or more separate accessory lobes apart from the main placental disc.
- Velamentous Cord Insertion: This is an abnormality where the umbilical cord, instead of inserting directly into the middle of the placenta, inserts itself into the foetal membranes and travels through them to reach the placenta.
- Previous C-Sections: Women who have given birth previously by C-section or have had other uterine surgeries are also at risk of developing vasa previa.
- Low-lying Placenta: If the placenta is low-lying, then it can also lead to vasa previa in pregnant women.
Symptoms of Vasa Previa
Mentioned below are the signs and symptoms of vasa previa:
- Unfortunately, vasa previa can go completely undetected until the mother goes into labour.
- One of the symptoms of vasa previa in pregnant women is painless vaginal bleeding from ruptured foetal blood vessels in the second or third trimester. The foetal blood will be dark red in colour.
- If your doctor detects that there is a rupture of membranes in your body, it could result in painless bleeding. It is one of the major symptoms of vasa previa.
- Foetal bradycardia is also a sign of vasa previa. It happens when the foetal heart rate becomes abnormally slow if the blood vessels rupture and start bleeding.
- If the mother has any of the risk factors mentioned earlier such as low-lying placenta, previous C-sections, IVF treatment, multiple foetuses, multi-lobed placenta, or abnormal cord insertion, the doctor will check for vasa previa during an ultrasound exam.
How Is Vasa Previa Diagnosed?
Vasa previa can be diagnosed by a transvaginal ultrasound along with a colour Doppler test. The doctor will recommend this if you have any of the risk factors or warning signs as mentioned previously. The vasa previa ultrasound can help in early diagnosis and timely management of the condition and ensure that the baby is safe and healthy.
Complications Associated With Vasa Previa
Vasa previa can be fatal for the foetus. It can also cause complications during delivery for the mother. The most common complication is that a C-section may have to be performed to deliver the baby safely.
A vasa previa C-section is elective if the condition has been diagnosed early in the pregnancy. When vasa previa has been diagnosed, the doctor recommends an elective C-section at 35 to 36 weeks to deliver the baby safely. If the mother goes into labour, the uterine contractions will rupture the blood vessels and cause the foetus to bleed out.
Vasa Previa Treatment
Vasa previa can be treated and managed if detected early in the pregnancy. Some of the treatment options include:
- Anti-contraction medication to suppress labour.
- Giving complete rest to your pelvic is important. It is suggested that you should not indulge in sexual intercourse and should not take vaginal exams, except transvaginal ultrasound. Complete bed rest is a must to avoid any physical strain.
- Hospitalization at 30 to 32 weeks is important to ensure that the mother and baby can be continuously monitored.
- Go for regular ultrasounds to make sure there is no rupture of blood vessels or bleeding.
- Steroid treatment for the foetus to speed up lung maturation can also be opted. This is because the baby has to be delivered by a C-section at 35 weeks. At 35 weeks, the baby is considered premature, and the lungs will not be fully developed.
- An elective C-section at 35 weeks can be done to avoid foetal blood vessel rupture.
How to Manage Vasa Previa
Vasa Previa can be managed in the following ways:
1. Antepartum
The antepartum period refers to the time period before childbirth. The antepartum care for vasa previa involves complete bed rest for the mother, especially in the last trimester. It also includes the use of labour suppressant medication to stop all uterine contractions, continuous monitoring of the foetus through transvaginal ultrasounds to make sure the umbilical cord is not compressed, and steroid treatment to speed up foetal lung maturation.
2. Intrapartum
Intrapartum refers to the time from the onset of labour until the delivery of the placenta. This period is usually avoided if the condition is diagnosed early. The doctor recommends an elective C-section at 35 weeks to avoid labour contractions that will rupture the cord blood vessels. If left undiagnosed and the mother goes into labour, the cord blood vessels will rupture from the contractions. This will cause the foetus to bleed and is mostly fatal. In such cases, the baby would have lost a lot of blood and has to be resuscitated and given a blood transfusion immediately to replace the lost blood.
3. Postpartum
This refers to the post-delivery period. The newborn baby’s umbilical cord needs to be clamped immediately to prevent blood loss. The baby needs to be checked immediately and may require a blood transfusion. The mother has to be checked for any signs of internal bleeding and needs post-surgical care.
Prognosis and Outcome
If detected early, the prognosis for vasa previa is good. If left undetected, it can be fatal for the baby, although it does not pose any health risks to the mother.
1. Neonatal Outcomes
When vasa previa is diagnosed prenatally, the foetus can be delivered via elective C-section and only 3 out of 100 babies born this way need a blood transfusion after birth. However, there may be complications for the baby related to premature birth such as underdeveloped lungs or low birth weight.
2. Long-Term Effect on Mother’s Health
Vasa previa does not pose any physical health risks to the mother apart from the risks of a C-section.
What Is the Survival Rate of Babies with Vasa Previa?
If diagnosed prenatally, the survival rate of babies is over 97%. However, if left undiagnosed, the mortality rate in babies is around 95%.
Vasa previa is very rare and occurs only in 4 out of 10,000 births. But it is a serious condition that can be fatal for the baby and hence needs to be diagnosed and treated early in the pregnancy. Consult your doctor if you have any risk factors for vasa previa mentioned in this article.
Also Read: Vaginal Bleeding During Late Pregnancy
Was This Article Helpful?
Parenting is a huge responsibility, for you as a caregiver, but also for us as a parenting content platform. We understand that and take our responsibility of creating credible content seriously. FirstCry Parenting articles are written and published only after extensive research using factually sound references to deliver quality content that is accurate, validated by experts, and completely reliable. To understand how we go about creating content that is credible, read our editorial policy here.