Heterotopic Pregnancy – Causes, Symptoms and Treatment
Understand heterotopic pregnancy, a rare condition involving simultaneous pregnancies, with insights on signs, risks, and medical management.

- What Is a Heterotopic Pregnancy?
- How Common Is It?
- Causes of Heterotopic Pregnancy
- Symptoms of Heterotopic Pregnancy
- Diagnosis of Heterotopic Pregnancy
- Treatment of Heterotopic Pregnancy
- Risks and Complications
- FAQs
Every pregnancy is unique, and some can be challenging or even dangerous. It is important to understand what kind of a pregnancy you have, as some pregnancies can be a challenge to see out to term, while others can lead to different problems. Having a difficult pregnancy may lead to dire consequences unless the correct kind of care is taken. One rare but serious condition is a heterotopic pregnancy. Similarly, heterotopic gestation requires prompt diagnosis to preserve the viable intrauterine pregnancy while addressing the ectopic component. Without timely intervention, both the parent and the intrauterine fetus face significant risks.
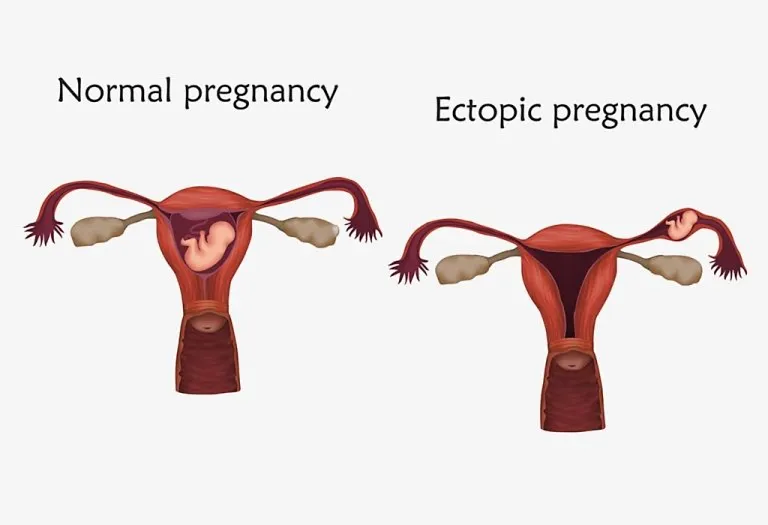
What Is a Heterotopic Pregnancy?
In the circumstance that a pregnancy has multiple foetuses, there can be a situation where one of these foetuses is outside the uterus and inside a fallopian tube. This is known as a non-viable Ectopic Pregnancy. The foetus that forms within the uterus is considered an intrauterine pregnancy. A pregnancy where both a non-viable ectopic pregnancy and an intrauterine pregnancy exist simultaneously (where one foetus is in the uterus, and another is outside) is known as a heterotopic pregnancy (1). This kind of pregnancy is rare but is as dangerous as an ectopic pregnancy, where only one foetus exists, and it is outside the uterus.
How Common Is It?
As mentioned above, this type of pregnancy is not common. According to doctors, any pregnancy that is part of natural conception or spontaneous conception, more commonly referred to as sexually viable pregnancies, is less at risk for heterotopic pregnancies. The chances of such a pregnancy occurring are 1 in 30,000 couples if neither partner was part of a heterotopic pregnancy, and 1 in 10,000 in couples that have a partner who may have been part of a heterotopic pregnancy during their infancy. In artificial conception methods like IVF or external conception methods like surrogacy pregnancies, the rate can drastically increase, but is still only 2 in every 1000 assisted pregnancies.
Causes of Heterotopic Pregnancy
The causes of heterotopic pregnancy can be hard to identify; doctors are still trying to understand what the root causes of this condition are. Here are a few known reasons that may lead to heterotopic pregnancies:
- History of the pelvic inflammatory disease can increase the risk of heterotopic pregnancies.
- Assisted pregnancies can cause this condition.
- Surgical treatments for infertility can cause this condition as a side effect.
- During IVF, the force generated due to the procedure can lead to this condition.
Symptoms of Heterotopic Pregnancy
As with any condition, it is crucial to understand what the signs and symptoms of this kind of pregnancy are. Here are some of the heterotopic pregnancy symptoms (2):
- Abnormal and excessive vaginal bleeding
- Severe or mild abdominal pain that is persistent during the pregnancy
- Pain on the sides of the upper torso that is constant and unbearable
- Extreme or unusual bloating
- Constant dizziness or lightheadedness
- Severe nausea
- Constant vomiting
- Vomiting blood
- Fainting on a regular basis

If you experience these signs and symptoms, please consult your medical professional immediately.
Diagnosis of Heterotopic Pregnancy
For a doctor to be able to come to a diagnosis of heterotopic pregnancy, certain guidelines and markers have to be considered. Here are a few of the guidelines (3):
- For the first three weeks of the pregnancy, doctors will monitor any suspected cases with blood tests.
- The most conclusive way of making a diagnosis can only happen through an ultrasound; this can only happen a month into the pregnancy.
- Routine urine tests may also help with the diagnosis.
- Although the symptoms can be clear, they can be part of multiple diagnoses until the ultrasound is done. The doctors will monitor and treat expectant mothers carefully if they suspect heterotopic pregnancy is a real risk.
Treatment of Heterotopic Pregnancy
Unfortunately, the risk that a foetus, that is outside the uterus, poses to the intrauterine pregnancy and the mother is incredibly high. This is why the only way to successfully ensure the survival of the mother and the other foetus is by terminating the outer foetus through surgery (4). Although this can be painful, the sad fact is that the other foetus has no chance of surviving if it is outside the uterus. Currently, there are no other heterotopic pregnancy treatment options.
Risks and Complications
Some couples face a dilemma of terminating the pregnancy, and understanding the risks and complications of attempting to carry the baby to term can help explain why this option is necessary. Most heterotopic pregnancy complications can be so extreme; it can lead to fatal outcomes for both the foetuses and the mother. At the very least, the chances of a miscarriage are extremely high; it can almost be considered a certainty. An additional risk is that carrying the foetuses to term could harm the mother’s body to an extent where she may never be able to live without assistance. One thing to consider here is that the foetus outside the uterus has no chance of survival. The uterus is an environment that is specifically designed to house and nurture a foetus, and a fallopian tube cannot do the same. In most cases, a mother can successfully deliver the intrauterine foetus in a healthy and safe manner.
FAQs
1. Can a heterotopic pregnancy be mistaken for a normal twin pregnancy?
Yes, in rare cases, a heterotopic pregnancy may be confused with a twin pregnancy because one embryo develops inside the uterus while the other grows outside it. This situation is sometimes referred to as a heterotopic twin pregnancy, which can delay accurate diagnosis. Early ultrasound helps clearly identify both implantation sites.
2. Why is a heterotopic gestation more likely in women who had pelvic infections or tubal surgery?
Scarring from infections or surgery can damage the fallopian tubes, making it hard for embryos to reach the uterus. After fertility treatments like IVF, one embryo may implant in the uterus while another gets stuck in a damaged tube. If undetected, this can lead to a ruptured heterotopic pregnancy, causing dangerous internal bleeding even while the uterine pregnancy remains healthy (5).
It is perfectly normal for mothers to undergo a depressive phase when the termination is done; this is why your medical specialist will recommend counselling. Even if the other foetus is successfully delivered, it is common and normal for the mother to grieve the terminated foetus. To help manage this loss, you can ask your doctor to help you find support groups and grief counsellors. It is important to see a psychologist and attend regular counselling sessions with your partner to help manage grief and loss.
Also Read:
Cramping in Pregnancy
Abdominal Pregnancy
Viable or Nonviable Pregnancy
Was This Article Helpful?
Parenting is a huge responsibility, for you as a caregiver, but also for us as a parenting content platform. We understand that and take our responsibility of creating credible content seriously. FirstCry Parenting articles are written and published only after extensive research using factually sound references to deliver quality content that is accurate, validated by experts, and completely reliable. To understand how we go about creating content that is credible, read our editorial policy here.