Harlequin Ichthyosis in Infants – Causes, Symptoms, Diagnosis, and Treatment
Ichthyosis is a group of disorders with persistently dry, scaly skin throughout the body. Autosomal recessive congenital ichthyoses (ARCI) are found in three major forms, Harlequin ichthyosis, lamellar, and congenital ichthyosiform erythroderma. Harlequin ichthyosis is the least common but most severe inherited form of ichthyosis affecting the skin of newborns.
What Is Harlequin Ichthyosis?
Harlequin ichthyosis is an autosomal recessive type of genetic disorder inherited from parents where both are carriers of the mutated gene ABCA 12. In the Harlequin disease, the newborn has thick skin with cracks and splits. These plates of thick skin can cause face distortion and breathing and eating problems. There is a need for immediate neonatal intensive care soon after birth for these infants.
The first case of Harlequin Ichthyosis was reported in 1970 by Reverend Oliver Hart. Currently, 70 disease-causing variants have been found. The other terms for the disease are Harlequin baby disease, Hyosis Fetalis, Ichthyosis Fetalis, Keratosis Diffusa Fetalis, Harlequin Fetus, Ichthyosis Congenital Gravior.
Who Is Prone to Harlequin Ichthyosis?
Harlequin Ichthyosis affects both gender types, i.e., males and females, equally. Consanguineous marriages (marriage between close relatives) have higher risks of getting this disease. Both the parents being silent carriers of autosomal recessive genes causes this disorder in the child. A newborn child or child in the womb is prone to Harlequin Ichthyosis. 1/500,000 persons are born with this condition in the US annually.
Causes of Harlequin Ichthyosis
Mutations in the Adenosine Triphosphate binding cassette sub-family A member 12 gene (ABCA 12) cause Harlequin ichthyosis disorder. This condition is passed through autosomal recessive parents and expressed when the baby inherits the affected gene from both parents. ABCA 12 gene codes for a transporter protein that carries out the transport of epidermal lipids across cell membranes. This gene plays a vital role in normal skin development. Mutations either prevent the formation of ABCA12 protein or form an abnormally small protein version that cannot transport lipids properly. Disruption in lipid transport leads to abnormality in epidermis formation and thus results in thickened skin all over the body.
If parents are carriers, 25% chances exist to transmit the disease to the kid. Also, there is a risk of 50% for the child to be a carrier when both the parents are carriers. Only in 25% of cases the kid receives normal genes from parents who are both carriers.
Symptoms of Harlequin Ichthyosis
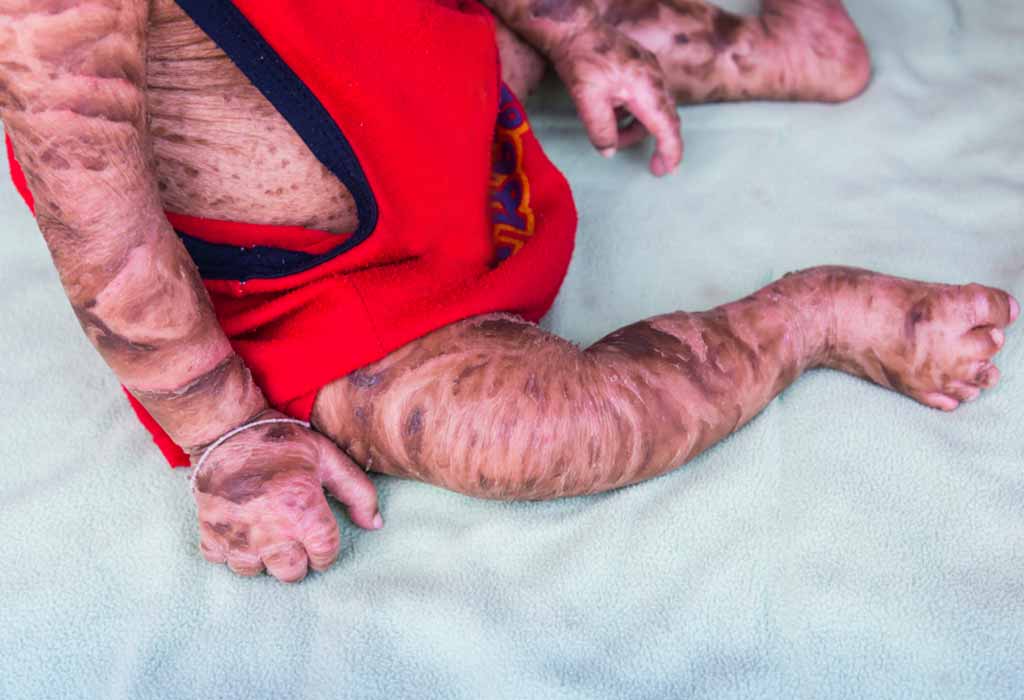
Children suffering from this condition show distinct changes in their skin, facial, and clinical features. Some of the Harlequin Ichthyosis signs include:
1. Skin Features
- Skin issues immediately after the baby is born
- Thick and hard skin all over the body
- Diamond-shaped plates of hyperkeratotic scales all over the body
- Erythematous fissures caused by the cracking of the scales
2. Facial Features
- Facial deformity due to pulling of the thickened skin occurs
- Poor development of the nose with nasal hypoplasia, eroded nasal alae, and obstructed nares
- Everted eyelids, which subject eyes to infections and dryness
- Eclabium due to dry skin
- Poor development of ear or absence of ears obstructing the external auditory canal
3. Clinical Features
- Limbs are covered with thick hyperkeratotic skin
- Presence of more fingers or toes than normal
- Incomplete development of digits and extra fingers and toes, clenched fists, incurved toes
- Restricted movement of arms and legs
- Thermal dysregulation due to thickened skin
- Disturbed sweat gland function that leads to heat loss mechanism disruption, increasing body temperature and heat strokes
- Loss of moisture from the body leading to dehydration
Harlequin Ichthyosis Complications
If Harlequin Ichthyosis is not detected prenatally, it causes several complications at birth that includes the below complications:
- Preterm birth of the child leads to death in the first few days of life
- Disrupted skin barrier exposes babies to life-threatening infections
- Restriction in chest wall expansion causes hypoventilation and respiratory failure, one of the primary causes of death
- Muscle shortening occurs due to hyperkeratotic skin near the joints
- Constricted limbs (fingers and toes), leading to Necrosis, swelling, and autoamputation
- Nursing difficulties due to the thick skin around the mouth, making it difficult to suck milk from their mother’s breasts
- Prematurity
How Is Harlequin Ichthyosis Diagnosed?
After the birth, the initial Harlequin Ichthyosis diagnosis is based on physical signs of harlequin ichthyosis. On confirming physical conditions related to the disorder, carry out other genetic tests for loss of function mutation in the ABCA12 gene.
If a person has a family history of ichthyosis, it is a must to check if you or your partner are carriers. If you are already pregnant, genetic testing with samples of skin, blood, or amniotic fluid is advised. Prenatal diagnosis (PND) with amniocentesis, Chorionic Villus Sampling, and ultrasound may support the diagnosis of mutation in ABCA12 in the early stages.
DNA-based diagnosis is recommended as they are reliable and conclusive. Preimplantation genetic diagnosis (PGD) can be a better option to avoid prenatal diagnosis. Preimplantation genetic diagnosis looks into the genes of the developing embryo, wherein in-vitro fertilization followed by testing sources before transferring to the mother’s womb is done. Genetic testing is the most specific method wherein loss of function mutation in the ABCA12 gene is diagnosed. Genetic testing has the limitation that it cannot give information on disease severity or prognosis.
On conducting a skin biopsy, look for a very thickened stratum corneum, parakeratosis, and hypergranulosis. Currently, a skin biopsy is not advised for prenatal diagnosis. As phenotypic expressions are expressed late, there is the missing or delayed diagnosis in prenatal scans.
Antenatal USG, specifically 3D type, is also an option in prenatal diagnosis but may be a challenge because of late phenotypic expression. Late phenotypic expression leads to late detection, making further management more difficult.
What Is Differential Diagnosis for Harlequin Ichthyosis?
A process wherein medical experts differentiate many medical conditions behind the symptoms present is known as Differential Diagnosis. These possibilities are then ruled out via genetic testing in diagnosing Harlequin Ichthyosis.
Mutations in ABCA 12 gene impairs the transport of lipids in the skin or form skinny versions of proteins involved in skin formation. Collodion membrane and congenital ichthyosiform erythroderma-like presentation are seen in a lesser degree of mutations. Based on these, differential diagnoses for Harlequin Ichthyosis are carried out.
Differential diagnosis is performed as below:
1. Inherited ichthyoses
Different mutations can cause congenital and delayed inherited ichthyoses in infants. Symptoms may be similar to harlequin ichthyosis.
- Ichthyosis Vulgaris: It contributes to 95% of ichthyosis and results from a mutation in the gene encoding filaggrin proteins. Filaggrin protein binds to keratin fibers for skin barrier formation that maintains pH. Skin dryness, Eczema is observed. Infants are prone to asthma and rhinitis later on after few months.
Recessive X-linked ichthyosis is the outcome of steroid sulfatase enzyme mutation. Steroid sulfatase is involved in the metabolism of cholesterol sulfate in the skin tissue, and its deficiency leads to the accumulation of cholesterol sulfate that damages the skin barrier. Skin scaling may gradually improve with time. - Autosomal recessive congenital ichthyosis: This class involves autosomal recessive inheritance, including Harlequin Ichthyosis (HI). This group also includes Lamellar ichthyosis resulting from TGM 1 mutation, Congenital ichthyosiform erythroderma from ALOXE3 mutations, and Netherton syndrome from SPINK5 mutation.
- Keratinopathic ichthyoses: Mutation in the Keratin gene leads to Keratinopatic ichthyosis. Classified into three types:
- Epidermolytic ichthyosis is caused by a mutation in KRT1 or KRT10 gene. Scaling of skin, redness, and blisters are observed.
- Superficial epidermolytic ichthyosis is caused by KRT2 mutation. Blisters and erosions are observed at birth.
- Ichthyosis Curth-Macklin is caused by KRT1 mutation. Skin Scaling across the body is observed.
2. Gaucher disease
It is an autosomal recessive inherited disorder of metabolism leading to glucocerebrosidase deficiency. In this case, Glycolipid glucocerebroside accumulation is observed.
Neuronopathic type of Gaucher’s disease (type 2) occurs in infants. Skin issues, such as collodion babies or sausage skin, are commonly observed. Premature birth is also observed, accompanied by peeling off of collodion membrane, which may happen in few weeks.
3. Sjogren-Larsson syndrome
Sjogren-Larsson syndrome falls under inborn error of metabolism. The deficiency of fatty aldehyde dehydrogenase enzyme in the body is responsible for regular oil and fat production in the skin.
Ichthyosis, speech disabilities, intellectual impairment, spasticity, or collodion baby can be the possible outcomes.
4. Trichothiodystrophy
Trichothiodystrophy is an autosomal recessive disorder that results in sulfur-deficient brittle hair. Developmental delay, photosensitivity, ichthyosis, or short stature are observed in such cases.
5. X-linked chondrodysplasia punctata
This disorder mainly affects male babies and is caused due to mutations in the ARSL gene encoding enzyme arylsulfatase E. Bone and cartilage development are affected. Short stature, short fingers and toes, alopecia, and ichthyosis are commonly observed.
Harlequin Ichthyosis Treatment
As soon as they are born, infants with harlequin ichthyosis require care from a multi-disciplinary team with doctors specialized in various subjects. One cannot cure harlequin ichthyosis completely but can take preventive measures to increase life span and health. These treatments focus on handling dehydration and electrolyte imbalances.
Usage of oral retinoids aids in extending the life span to a great extent. Oral retinoids have toxicity and side effects, so they are used only in severe cases. Thus, it is crucial to keep a harlequin ichthyosis newborn in neonatal intensive care in a heated incubator with high humidity and hygienic handling while supplying nutrients via tube feeding. It is essential to lubricate the eyes of a newborn with eye drops to keep them healthy. Using protective devices to protect their eyes is also important. You can apply retinoids to help shed hard skin that peels off in few weeks. Antibiotic treatment and one-on-one nursing care are also important for the newborn to prevent infection at this time.
Insert a tube airway for breathing and keep the skin moisturized after showering with cholesterol, lanolin, and petrolatum products. Remove collodion membrane on digits and thorax to maintain circulation and adequate respiration.
Carry out physical examination regularly for infection, skin involvement, and skin malignancy. Make relaxation incisions to prevent digital autoamputation or Necrosis. Several investigational therapies are being conducted for treatment solutions of harlequin ichthyosis. The US Government funding and private industries are supporting these investigations.
Outcomes of Harlequin Ichthyosis
The disorder was considered fatal in previous decades as the infants hardly survived more than a few days. Although harlequin ichthyosis requires careful monitoring, skin protection, and topical treatments, the therapy outcome has increased compared to earlier times. Neonatal intensive care, oral retinoids, Isotretinoin has shown promising results. The case requires ophthalmologists, dermatologists, surgeons, dieticians, clinical geneticists, genetic counselors, and psychologists to work together for betterment.
Patients still have issues with thermoregulation, poor hair growth, scaly skin, alopecia, digit contraction. The number of survivors is increasing, giving a better outlook of the current treatment strategy. However, the situation can improve if proper social and psychological support is provided. Skin lubrication should be advised. It is important to make parents aware of the signs of this disorder. If groups of parents with kids with similar issues connect on social media, it will help to heal their emotional imbalance.
(Fun Fact: 1984 born Nusrit ‘Nelly’ Shaheen is the oldest harlequin ichthyosis survivor with better health conditions.)
Also Read:
Craniosynostosis in Infants
Tay-Sachs Disease in Infants
CHARGE Syndrome in Infants
Was This Article Helpful?
Parenting is a huge responsibility, for you as a caregiver, but also for us as a parenting content platform. We understand that and take our responsibility of creating credible content seriously. FirstCry Parenting articles are written and published only after extensive research using factually sound references to deliver quality content that is accurate, validated by experts, and completely reliable. To understand how we go about creating content that is credible, read our editorial policy here.
















.svg)


















