Choriocarcinoma: Causes, Signs & Remedies
Choriocarcinoma is a rare and rapidly growing malignant cancer that occurs in the uterus after a molar pregnancy. It falls into the category of gestational trophoblastic disease. It can arise in women who have had a miscarriage, or an ectopic pregnancy. It can also occur in normal pregnancies. However, a hydatidiform mole is the main cause of the disease. Read on to know more about choriocarcinoma.
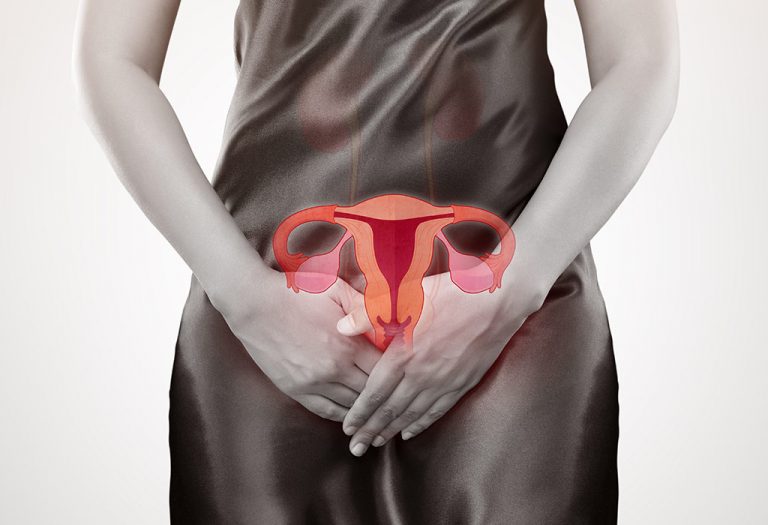
What Is Choriocarcinoma?
Choriocarcinoma is a malignant tumour. It mostly occurs in the placenta of pregnant women. The cancerous cells first develop in the tissue of a developing placenta. However, in some rare cases, it forms in men’s testicles and in the uterus of the affected post-menopausal woman.
How Common Is It During Pregnancy?
Choriocarcinoma is relatively rare with an incidence of one case per 40,000 pregnancies and for it to occur during pregnancy is even rarer. Studies suggest that about one in every 40,000 pregnant women and one in 40 patients with hydatidiform moles are likely to develop the disease in America and Europe. The number increases in Southeast Asia and Japan; about 9 in 40,000 pregnancies, and 3 in 40 patients with hydatidiform moles are likely to develop it in these regions. And, one in every 2800 pregnancies in China are likely to be affected by it.
What Causes Choriocarcinoma?
- Choriocarcinoma after a normal pregnancy may occur, but it is more prevalent during molar pregnancy. The disease comes into being when big lumps called hydatidiform moles are formed in the uterine tissue at the beginning of a pregnancy. These moles then become cancerous, and the cells start multiplying. Then they start spreading out.
- Choriocarcinoma may also affect people who have had a miscarriage or an ectopic pregnancy (which occurs outside the womb).
Who Is Most at the Risk of Getting Choriocarcinoma?
The following women are most at the risk of choriocarcinoma:
- Women who get pregnant before 20 or after 40 are at a greater risk of acquiring the disease.
- Women who have experienced any prior incident of molar pregnancy.
- A person with low levels of carotene and Vitamin A in her diet is at risk of molar pregnancy which in turn could trigger choriocarcinoma.
- People who belong to blood groups of A or AB.
- Rarely there have been few incidences of more than one woman from the same family suffering from a molar pregnancy.
What Are the Symptoms?
The signs and symptoms of choriocarcinoma are given below:
- Lumps in the uterus.
- Continuous vaginal bleeding.
- Cysts present in the ovary.
- High HCG levels during and after the first trimester.
- Hypogastric pain.
- If in case the cancer cells have spread to the lungs, then the person may experience shortness of breath, chest pain, and may cough up blood.
- Increase in thyroid-stimulating hormone (TSH).
- In some people, the signs of the disease may be apparent, but some people may be asymptomatic.
Stages of Choriocarcinoma
Choriocarcinoma, also referred to as uterine choriocarcinoma, had the FIGO staging system, which is as follows:
- STAGE I: The disease is limited to the uterus.
- STAGE II: It then starts spreading and is limited to the female genital tract only.
- STAGE III: It starts spreading upwards towards the lungs.
- STAGE IV: In this stage, all the metastases spread to the other parts of the body. Being hematogenous in nature, the metastases spread in other parts of the body through blood circulation.
How Is the Diagnosis Made?
Choriocarcinoma can be diagnosed and detected firstly through lumps in the uterus. However, lumps or oedema may not be detected in all cases. The HCG level is tested, and in this disease, it is noticed that it becomes very high. Apart from this, the doctor may recommend a kidney test, a liver test and a complete blood count test. A CAT scan, a CT scan or an MRI are more specific tests in locating internal abnormalities. To detect any attack on the lungs, the doctor will ask for a chest x-ray. The doctor also does a thorough examination of the pelvis to check the condition of the uterus.
Complications
The Complications of choriocarcinoma include:
- Hyperthyroidism
- A rise in HCG level (Serum)
- Uterine enlargement
- Intermenstrual PV Bleed
- Spread of cancer
Treatment for Choriocarcinoma
Treatment for choriocarcinoma is according to the stage of cancer. If a tumour is small and has not spread to other parts of the body, it is low-risk. Such tumours can be cured by chemotherapy alone. In case the tumour is big and has spread to other parts of the body, then it will be considered high-risk and will require surgery and chemotherapy, or surgery, chemotherapy and radiation.
1. Chemotherapy
Except for a tumour in the testicles, choriocarcinoma reacts well to chemotherapy.
2. Surgery
Surgery in choriocarcinoma includes removal of uterus or hysterectomy. This is usually done for women above 40 years.
3. Radiation Therapy
Radiation treatment is for people who are at high risk. It is given at a time when the cancer cells have spread to other parts of the body.
4. Hysterectomy
Choriocarcinoma is usually treated with chemotherapy. In case the tumour is chemoresistant, i.e. it cannot be cured by chemotherapy, then the womb is removed to get rid of the disease.
Can You Get Pregnant?
The high levels of HCG may stop your periods. It may again start after a while, and the cycle may become normal; however, after chemotherapy, it will again stop. Your cycle will again get back to normal after 3-6 months after your chemo stops. However, it is to be understood that if hysterectomy (removal of the womb) is done in women with choriocarcinoma, they will never be able to get pregnant again.
The Prognosis (Outlook)
- In the case of cancer not having spread to other parts of the body, the woman has every chance of conceiving again.
- The cancer is hard to cure if it has spread to the liver or the brain.
- In case cancer recurs again despite the person being given chemotherapy earlier, it is hard to cure it.
- If the person gets affected after she delivers, then it can have chances of not getting cured.
- About 70% of women after treatment get cured and go into remission (disease-free).
Prevention
- Early detection of choriocarcinoma can lead to positive outcomes and maximize the chances of cure with chemotherapy.
- The HCG levels should be regularly monitored for a year after undergoing chemotherapy.
- Early adequate treatment can increase the chances of a full cure of the disease.
- Pregnancy should be avoided during chemotherapy and also the first year after chemotherapy stops.
- Having nutritional food goes a long way in preventing the disease.
The association of cancer with pregnancy is on the increase. Although chemotherapy is considered to be the best treatment for choriocarcinoma, it can pose a danger to the foetus. Also, in case a woman has to undergo a hysterectomy, it can be emotionally challenging for her since conceiving after that will not be possible. Also, too much delay in treatment could result in the disease spreading to the other parts of the body. Therefore, the most viable thing would be to treat the disease in its early stage.
Was This Article Helpful?
Parenting is a huge responsibility, for you as a caregiver, but also for us as a parenting content platform. We understand that and take our responsibility of creating credible content seriously. FirstCry Parenting articles are written and published only after extensive research using factually sound references to deliver quality content that is accurate, validated by experts, and completely reliable. To understand how we go about creating content that is credible, read our editorial policy here.