Molar Pregnancy: Causes, Signs & Treatment

Molar pregnancy is a rare pathological condition of the cells that form the placenta seen in pregnant women. The fertilised egg or the embryo fails to develop, and is replaced by a pathological grape-like cluster (mole).
What Is A Molar Pregnancy?
A molar pregnancy is one in which, after fertilization, the embryo is abnormally developed and appears like a bunch of grapes, called a hydatidiform mole. It is a rare developmental disease of the cells that form the placenta, and is usually detected in the early trimesters and in most cases, results in wasted pregnancy.
Types

Based on the genetic and chromosomal pattern, molar pregnancies are divided into complete and partial molar pregnancy.
- Complete Molar Pregnancy: During fertilisation, 23 chromosomes each are received from the mother and the father, and the fertilised egg hence contains 46 chromosomes altogether. In a complete molar pregnancy, the 23 maternal chromosomes are missing, and the embryo consists of only 23 chromosomes that are paternal in origin. This leads to the absence of foetal growth and formation of abnormal cysts, which appear like grapes.
- Partial Molar Pregnancy: In a partial molar pregnancy, the embryo consists of 23 maternal chromosomes, but these chromosomes are fertilised by double the number of paternal chromosomes, 46 instead of 23. This leads to a total constitution of 69 chromosomes. The resultant embryo may grow and develop into an immature foetus, which may not survive beyond the few initial months of intrauterine growth due to the unfavourable genetic makeup.
Causes
The cause of the genetic abnormalities is largely unknown. However, the following factors have been associated with an increased risk for molar pregnancy:
- Extremes of Age: It is more common in teen pregnancies and those after the age of 40.
- Ethnic Origin: It is twice more common in women of Asian origin.
- Past History: Women with a history of molar pregnancy in the past, are at an increased and proportionate risk. One such pregnancy in the past, predisposes to a risk of 1-1.5%, while two or more such past pregnancies increase the risk to 15-20% chances of having a molar pregnancy again.
Risk Factors That Can Increase the Possibility of Molar Pregnancy

Molar pregnancies are associated with certain risk factors including:
- Diet: Deficiency of carotenes or vitamin A.
- Genetic disorders: Women with pre-existing genetic or chromosomal diseases.
- Other gynaecological disorders: for example, history of the polycystic ovarian disease (PCOD).
- Radiation exposure: Genetic diseases are more common with excessive exposure to radiations for imaging or therapy.
How Common Are Molar Pregnancies?
Worldwide, the condition is more common in women from the Asian subcontinent where it occurs at a frequency of 1 in every 1500 pregnancies. It is also more common in women who had a molar pregnancy in the past.
Signs and Symptoms
A molar pregnancy may be asymptomatic or present with the usual symptoms of a normal pregnancy in the early few days. With advancing gestational age, it may present with the following symptoms:
- Abnormal vaginal bleeding: first or early second trimester.
- Disproportionately large uterus: large cysts may be present.
- Metabolic and gastric symptoms: nausea and vomiting.
- Autonomic instability: hypertension, sweating, palpitations, diarrhoea, etc.
- Discomfort or dull pain in the lower pelvis.
- Small cysts or clusters of grape-like substance from the vagina usually suggest molar pregnancy. This symptom is specific for molar pregnancy.
However, these symptoms are highly non-specific (except the last one) as they may also occur in normal pregnancy or the case of a miscarriage.
How Is the Diagnosis Made?
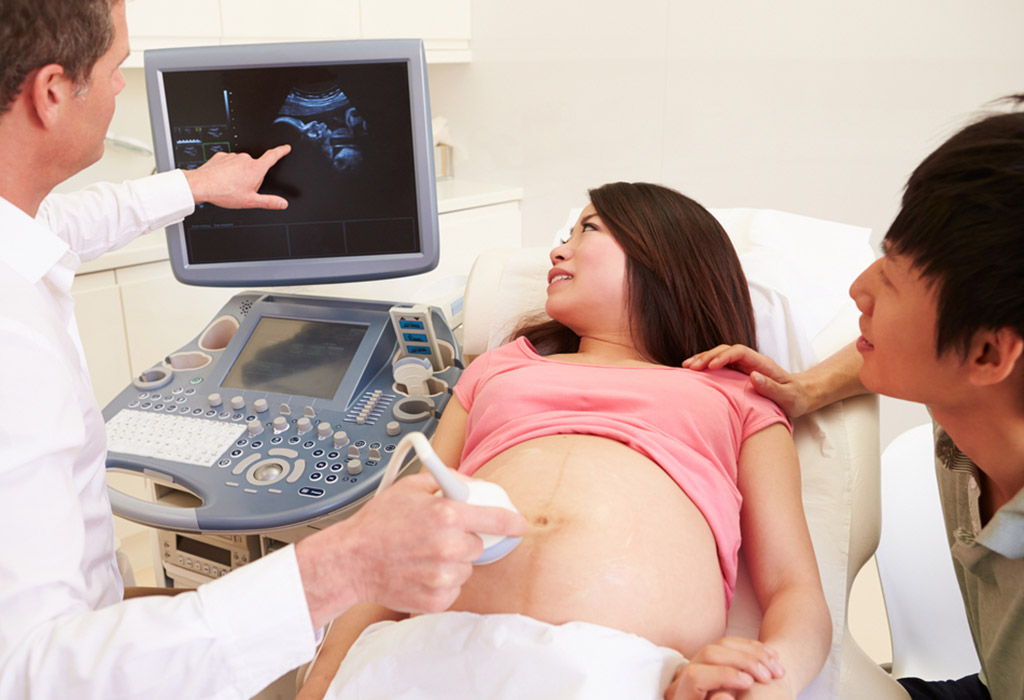
Diagnosis of molar pregnancy can be based on laboratory studies and imaging studies.
- Beta HCG (human chorionic gonadotropin) levels: It is a hormone secreted by the placenta soon after fertilisation of the ovum during pregnancy. It can be measured in the blood as well as the urine. In a normal pregnancy, the levels range between hundreds (IU/ml) and proportionately increase with increasing gestational age. In molar pregnancies, the levels of B-HCG are enormously raised, exceeding 100000 IU/ml in few cases.
- Molar pregnancy ultrasound: It is the investigation of choice for the diagnosis and confirmation of a molar pregnancy. An ultrasound shows a ‘snowstorm pattern’ with multiple cysts like growths in the uterine cavity and an absence of foetal activities. It is the safest, quickest and most reliable diagnostic tool for a molar pregnancy. It also confirms the diagnosis made by abnormally high beta HCG levels.
Risks and Complications
Molar pregnancies can be associated with the following risks and complications:
- Invasive mole or choriocarcinoma: Complete molar pregnancies can progress to invasive mole or choriocarcinoma.
- GTN or Gestational Trophoblastic Neoplasia: Molar pregnancies are associated with a risk of conversion to trophoblastic malignancy in the future. These are localized malignant conditions with a fairly good prognosis.
- Recurrence: A history of molar pregnancy increases the risk for recurrence of this condition.
- Foetal loss: Complete moles usually result in foetal loss. Women with molar pregnancies are at a high risk of miscarriages and other pregnancy-related complications as the genetic makeup of the foetus results in its premature death.
Treatment
- Suction Removal or Dilation and Curettage(D&C): When a molar pregnancy is suspected by symptoms, hCG levels or ultrasound, a Dilation & Curettage is usually undertaken. It simply involves dilation of the cervical canal and suctioning the entire contents or spooning or curetting of the uterine contents to histopathologically confirm the diagnosis and therapeutically remove all the trophoblastic tissues.
- HCG Monitoring: In a few cases after treatment, some residual tissues are left behind in the uterine cavity after a D&C. This is correlated with serial monitoring of beta HCG levels, which ideally should start falling after treatment. In majority cases, the residual tissues are successfully treated with However a fraction of cases progress to gestational trophoblastic neoplasia.
- Medication: Medical treatment of molar pregnancy includes:
- Symptomatic therapy: correction of anaemias, anti-thyroid drugs.
- Antineoplastic drugs: drugs like methotrexate are useful in gestational trophoblastic neoplasia.
- Folic acid: supplements with high amounts of folic acid.
- Hysterectomy: For women with advanced age, or completed family or recurrent severe disease despite optimum medical therapy, hysterectomy is the best-suggested treatment option.
Monitoring After the Treatment
To avoid any residual disease, monitoring after treatment is essential. Regular follow-ups with your clinician after treatment, for serial physical examinations and history, are vital.
Beta hCG levels are the best means of monitoring after treatment with the help of serial monthly blood and urine tests. Normally, the very high molar pregnancy hCG levels should fall significantly after treatment. If it persistently remains high, residual or recurrent disease should be suspected. Screening ultrasound can be performed to rule out any possibility of trophoblastic disease after treatment.
Further Treatment After Molar Pregnancy
Despite curative treatment available for molar pregnancy, a few cases (1% partial and about 15% complete) may have a residual tissue, and this is known as a persistent trophoblastic disease (PTD). It may have malignant behaviour with spread to other body tissues, commonly involving the lungs. Treatment involves chemotherapy with methotrexate cycles along with folic acid supplementation.
Prevention

Since the pathophysiology is largely genetic, no definite preventive measures are available. However, following steps can be considered:
- Balanced diet: include adequate carotene and other green vegetables in your daily diet.
- Avoid cigarette smoking and alcohol consumption.
- Avoid conceiving for at least a year after previous molar pregnancy.
- Consult a genetic counsellor and consider gene studies and chromosomal mapping.
Chances of Molar Pregnancy In Future
Molar pregnancies have a 1.5-2% risk of recurrence. No serious long-term health hazards are reported. One may have a normal pregnancy after a molar event. However, a gap of six months following surgery and about a year after chemotherapy is advisable before conceiving to avoid recurrence.
When Can You Try to Get Pregnant?
Fortunately, molar pregnancy or its treatment does not affect the fertility. Also, it has a low (1.5-2%) risk of recurrence. Clinicians worldwide advice a waiting period of 1 year before conceiving. This gives time for the beta hCG to return to the physiological levels. Once pre-pathological levels are recorded, you may now plan a safe pregnancy.
How to Cope With Fear and Loss
A molar pregnancy can be a traumatising experience, and a grave loss of your child like in miscarriages. Strong will power and your partner’s support is vital. Undue anxiety and over treatments to avoid recurrence can be dangerous. Consulting a counsellor and considering adoption are advisable.
Molar pregnancy is a rare pathological condition that involves loss of pregnancy. With a good understanding of molar pregnancy meaning, timely evaluation, and complete treatment, this condition can be managed, and its recurrence prevented.
Was This Article Helpful?
Parenting is a huge responsibility, for you as a caregiver, but also for us as a parenting content platform. We understand that and take our responsibility of creating credible content seriously. FirstCry Parenting articles are written and published only after extensive research using factually sound references to deliver quality content that is accurate, validated by experts, and completely reliable. To understand how we go about creating content that is credible, read our editorial policy here.



































