Patent Ductus Arteriosus – Causes, Symptoms, and Treatment
Patent ductus arteriosus is one of the most prevalent congenital heart deformities that is found in days or weeks after the birth of a baby. Doctors can detect this condition at birth and treat it. In most cases, the treatment is successful and restores the heart to its normal functioning. However, in rare cases, the defect can go undetected and may exist in adulthood if left untreated.
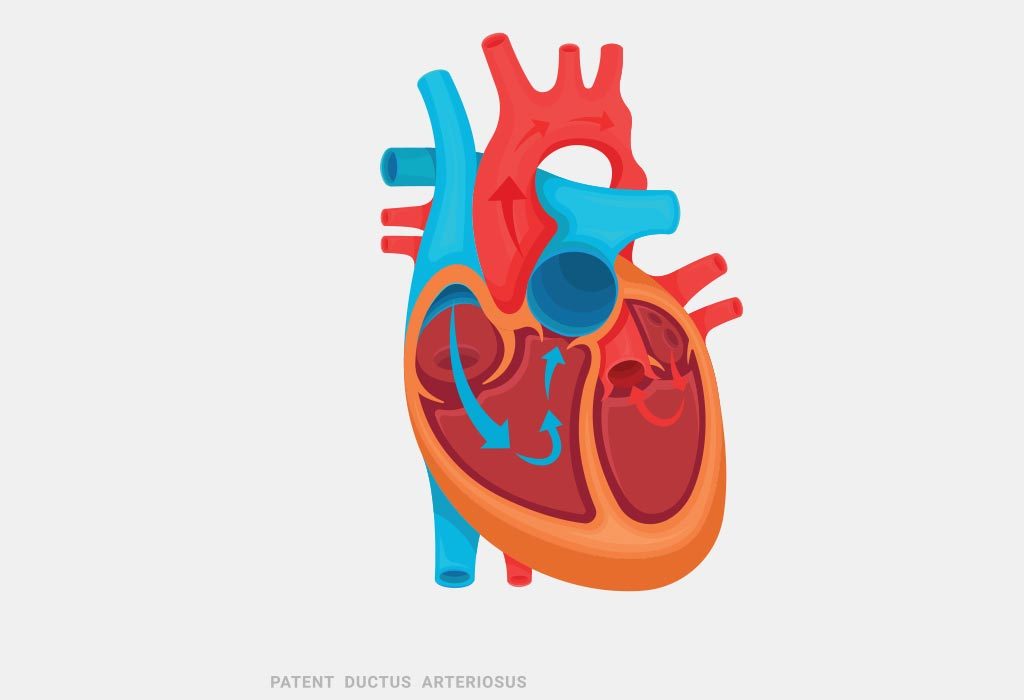
What Is Patent Ductus Arteriosus?
Patent ductus arteriosus is an auxiliary blood vessel that is found in the baby before birth and immediately after birth. In most cases, where babies have a normal heart rate the patent ductus arteriosus closes on its own just after a few days of birthing. But in case of the patent ductus arteriosus condition, this temporary blood vessel doesn’t close on its own after the birth of the child. If the PDA doesn’t close, then it may cause an increase in blood flow to the lungs than actually required. The symptoms may be severe or minimal depending upon the size of the PDA. The problem occurs only if the opening of the blood vessel is large; a smaller opening will close on its own by the time the child is about a year old.
What Causes Patent Ductus Arteriosus?
Patent ductus is considered to be a congenital heart defect that’s fairly common in newborn babies, however, the exact cause for the same is still not clear. This medical condition is more prevalent among girl babies and it is believed that genetics may play a major role in the cause. Premature babies, babies with a respiratory disorder, Down’s syndrome, and other genetic disorders are at a higher risk of developing PDA. At times, it also affects babies whose mother had been infected with rubella, a sort of German measles during the course of pregnancy.
Signs and Symptoms of Patent Ductus Arteriosus
The symptoms of patent ductus arteriosus depend upon the opening in the ductus arteriosus. It can be small or large, and accordingly, the symptoms will be mild or severe. If the opening in the ductus arteriosus is tiny then apparently there won’t be any symptoms and the doctor will be able to determine the defect only by hearing a distant heart murmur upon examination. But in case of a large PDA, the following signs and symptoms may be noticed in babies:
- Heavy and rapid breathing
- Extreme fatigue
- Increased heart rate
- Poor appetite
- Extreme sweating
- Shortness of breath or complete breathlessness
- Poor weight gain
- Infections
In certain rare cases, if the PDA goes undetected then as an adult you may experience frequent shortness of breath, heart palpitations, an enlarged heart, congestive heart failure or high blood pressure in the lungs.
Complications Associated With Patent Ductus Arteriosus
In most of the cases, PDA is diagnosed soon after the birth of the baby and can be treated successfully. In extremely rare cases, PDA might go undetected in adulthood which may cause several health problems depending upon the size of the opening. Some of the complications associated with PDA include:
- Frequent heart palpitations and extreme shortness of breath.
- A bacterial infection causing inflammation in the lining of the heart, also termed as endocarditis. It is more common with people having structural heart defects.
- High blood pressure in the lungs also termed as pulmonary hypertension. This complication can cause severe damage to the lungs.
- In extremely rare cases, PDA may cause congestive heart failure. This happens due to the extra blood flow to the heart that may cause heart enlargement and weakening of its muscles that eventually affects the ability of the heart to pump the blood effectively.
How Is Patent Ductus Arteriosus Diagnosed?
PDA is generally diagnosed soon after the birth of the baby by the doctor through a physical examination. In most cases, the heart causes a slight murmur or an unusual sound in the heartbeat which can be heard with the help of a stethoscope. The doctor refers to a chest X-ray to confirm and check the condition of the baby’s heart and lungs. In case of premature babies, they may not have the same symptoms as full-term birth babies and may require additional tests to confirm the condition. The diagnosis for PDA can be done by:
1. Chest X-Ray
A chest X-ray of a PDA infected child will clearly show if the child has an enlarged heart and any changes in the lungs.
2. Echocardiogram
An echocardiogram is one of the most common ways to diagnose PDA. It uses the sound waves to create a live image of the heart and heart valves. It shows the blood flow pattern of the heart and also determines how big the opening of the ductus arteriosus is and how much blood is passing through it.
3. Electrocardiogram
An electrocardiogram or an EKG shows the electrical activity of the heart and also detects any irregular heart rhythms. When conducted on infants, it can also identify an enlarged heart.
Treatment Options for Patent Ductus Arteriosus
The treatment of PDA depends upon the size of the opening of the ductus arteriosus, if the opening is too small then it may not require any surgical treatment. The valve will close on its own as the child grows older, in such cases, your doctor may regularly monitor the PDA as the baby grows. In case, it doesn’t close on its own then medication or patent ductus arteriosus surgery may be required. The treatment options for PDA include:
1. PDA Surgical Treatment
Surgery may become necessary if the opening is large and does not seal on its own. Surgical treatment for PDA is recommended only to infants who are at least six months old. The doctor may prescribe antibiotics after the surgery to prevent any bacterial infection.
After the surgery, the medical team will assist you with how to feed and give medicines to your baby correctly. You will also be guided on what symptoms you should report to the doctor. After the surgery, the doctor may prescribe pain medication such as ibuprofen or acetaminophen to keep your baby comfortable. In most cases, your child will recover fully within a few weeks of the surgery and can resume normal activities. Infants who used to get tired while feeding before the surgery will now be more energetic post-recovery. Feeding would get back to normal and the baby will start gaining weight.
2. PDA Medication
PDA medication is more effective in newborn babies, as and when the baby gets older more treatments may become necessary. For premature babies having PDA, a medication termed as ‘indomethacin’ is given to help seal the opening. This medication is given intravenously to help constrict the muscles and close off the duct.
3. Catheter-Based Treatment
The doctor recommends a catheter-based treatment if your baby has a PDA with a smaller opening. This treatment is done under sedation and does not involve the opening of the child’s chest as done in other surgical treatments. A thin flexible tube known as a catheter is inserted through a blood vessel from the groin area and guided into the child’s heart. A dye will be injected into the catheter to ensure that it is at the right place. A tiny coil or blocking device is passed through this catheter into the child’s heart that is placed on the PDA, which blocks the blood flow through the additional vessel and normalises the blood flow pattern of the heart. Once the blocking device is in the correct position it will be released from the catheter and the catheter will be removed. This treatment can be performed on infants who are at least 6 months old and weigh 22 pounds or more.
Nutrition Supplements for Infants With PDA
The babies born with PDA heart eat and grow normally in most cases. Some of the premature babies and infants with larger PDA opening may get tired quickly while feeding and may experience difficulty in gaining weight. The recommended nutrition for infants affected with PDA include:
1. Tube Feeding Supplements
In this case, supplements are given through tiny flexible feeding tubes that are inserted through the nose, pass down through the oesophagus, and into the stomach. Supplement feeding can be done through feeding bottle as well. Infants can be fed through the feeding bottle as much as they can take and the rest can be fed through the feeding tube. Some babies who get extremely tired when bottle-fed will be fed the breastmilk or formula milk through the feeding tube.
2. High-Calorie Supplements
Special high-calorie supplements will be added to the formula milk or breastmilk to enhance the intake of a number of calories. The breastmilk can be pumped if the baby cannot be fed directly. The high-calorie supplements make sure that your baby intakes enough calories required for their growth even if they drink less milk.
When to Consult a Doctor
You must contact the doctor immediately in the following cases:
- If your child has difficulty in eating and isn’t gaining weight normally.
- If your child gets tired easily while doing normal activities like playing or eating.
- If your child is always panting or experiences shortness of breath.
- If your child experiences breathlessness while eating or crying.
Prognosis
The long-term outlook of PDA is quite positive when diagnosed and treated soon after the baby is born. The recovery rate of full-term babies and children is quite high; for premature babies, the recovery would depend on how early the baby was born and if there are any other health issues present. In most cases, infants make a complete recovery from fetal patent ductus arteriosus without experiencing any negative effects.
PDA is a very common congenital heart defect that can be diagnosed and treated effectively without any complications. The treatment options as stated above have high success rates and the child can lead a normal and healthy life as he gets older. It’s important to speak to your baby’s cardiologist regarding his situation before deciding on the treatment line.
Also Read:
Tay-Sachs Genetic Disorder in Infants
Common Health Problems and Diseases in Infants
Biliary Atresia in Infants
Was This Article Helpful?
Parenting is a huge responsibility, for you as a caregiver, but also for us as a parenting content platform. We understand that and take our responsibility of creating credible content seriously. FirstCry Parenting articles are written and published only after extensive research using factually sound references to deliver quality content that is accurate, validated by experts, and completely reliable. To understand how we go about creating content that is credible, read our editorial policy here.



















.svg)


















