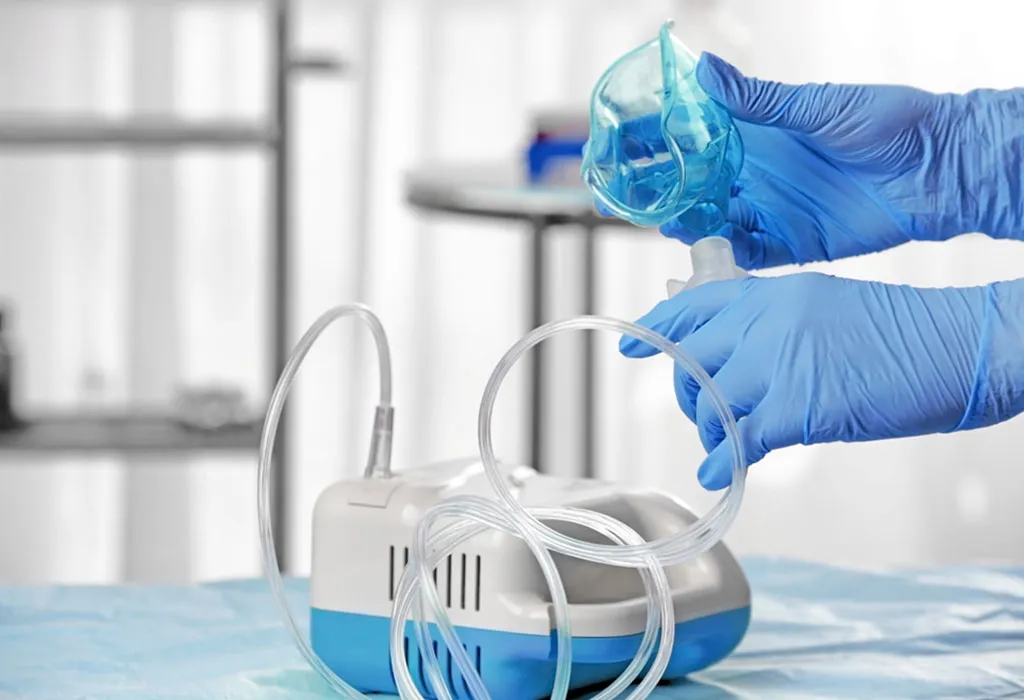
Nebulisation for Babies and Kids

You may have seen kids or babies having plastic masks around their faces during a check-up in a clinic, or hospital visit. These are called nebulisers, which assist a kid in breathing properly and the treatment is called nebulisation. A nebuliser for kids is a special device that warms or otherwise changes a liquid solution into a fine mist that’s easy to inhale. It is also known as breathing matching by some people and doctors often recommend these for kids and babies. With the help of a nebuliser, children take in medication while breathing as they normally would. Let’s learn more about this with the help of the article below.
What Is Nebulisation?
In simpler words, nebulisation is a type of a treatment that assists breathing. In this, the medication that a child requires is directly administered through the nebuliser and inhaled by the kid, so that it reaches the body easily and is absorbed quickly for immediate effect.
Is It Safe for Children?
Nebulisation is perfectly safe for most children. This treatment is only initiated once the doctor has checked your child and is sure that nebulisation is the way ahead.
What Is a Nebuliser?
A nebuliser is a machine that carries out the process of nebulisation. The medication required by the kid is administered by the machine to the child, usually through a nebulisation mask.
When to Use Nebuliser?
Here are some tips to use a nebuliser.
- Gather the Things: Wash your hands and collect the nebuliser and all the things you will need – mask, medicine, dropper, medicine cup, attachment tube, etc., and place the device on a flat surface.
- Position: Sit in a comfortable place and hold your little one on your lap in an upright position.
- Breathe: Through Nebuliser, After assembling the nebuliser and making your baby wear the mask, turn it on and make your baby breathe normally for five to ten minutes. Keep them distracted by showing them their favourite toy or reading from a book.
How Does a Nebuliser Work?
When using a nebuliser for kids, the medication is added to the machine. The nebuliser then uses the medication and converts it into an aerosol or a form that contains aerial droplets of the medicine. This combination of gas and liquid is achieved by making use of oxygen, ultrasonics, or air compressed by the machine. Once the aerosol is ready, it is let out through the nebulisation mask, which is put on the child.
Types of Medicines Used for Nebulisation
There are two types of medications generally used for nebulisation. They are,
1. Non-Medicated Liquid
When a kid has a dry nose and his mucous membrane must be moistened, nebulisation can be conducted using a simple saline liquid instead of medicine. This gently wets the membrane and reduces dryness.
2. Medicated Liquid
Kids suffering from rhinitis, asthma or similar diseases, are advised to take nebulisation by making use of medicated liquids that contain the chemicals required to treat the disease. In cases of severe asthma, corticosteroids or a combination of bronchodilators might be used in the medicated liquid and administered via nebulisation.
3. Inhaled Antibiotics
Some antibiotics are available via nebulizer treatment, like TOBI – a form of tobramycin used to treat certain bacterial infections.
How Often Can You Nebulise Your Child?
There is no generalised answer to the number of times a child must be nebulised. At times, a couple of doses might suffice. At times, the nebuliser dose for infants might have to be more frequent, depending on the problem and its severity. Doctors suggest keeping a nebuliser handy since administering medication quickly is essential in such cases. Its better be in touch with your child’s doctor about the dose frequency of the medicines.
How Can Nebulisation Help Your Child With Cold and Cough?
In case of a usual cough and cold, the nose tends to get dry from the inside and become extremely stuffy. This leads to a blocked nose and children begin to breathe from their mouth.
Using a nebuliser with a simple saline solution helps moisturise the inner nose membrane. This loosens any mucous that is trapped within and dilates the nasal passage. This is the quickest way to get relief from a blocked nose and the child can start breathing normally, very soon.
Should I Purchase a Nebuliser?
The severity of your child’s problem, his frequency of requiring nebulisation, the expense, comfort, and so on, play a vital role in deciding whether a nebuliser is needed at home. Opting for nebulisation in clinics and hospitals is always helpful since it comes with the care and guidance of the hospital staff. When a disease requires a few rounds of nebulisation at most, such an option is beneficial and cost-effective.
Having your own nebuliser ensures that kids can carry it out in the safety of a known environment. Also, if repeat administration of the medicine is required, a home nebuliser is best and works out to be more affordable.
What Are the Different Types of Nebulisers?
There are several types of nebulisers available in the market. Depending on your child’s condition, the doctor can recommend the best nebuliser for kids.
1. Stationary Nebulisers
- Usually sturdy, durable, and long-lasting.
- Quite cheap with a pretty long warranty.
- Generally meant to be used inside the house only.
2. Mobile Nebulisers
- Used in a handheld manner.
- Powered via batteries or other sources.
- Can be carried around and used while outside.
- Small in size and lightweight.
3. Ultrasonic Nebulisers
- Makes use of vibrations at a high frequency to convert liquid medicine to aerosol.
- Do not make a sound.
- Small in size.
- Battery operated, yet fast functioning.
4. Jet Nebulisers
- Push air through a plastic mask that converts liquid medicine to air form.
- Powered by electricity so not suitable to carry while travelling.
- Makes a loud sound, but quite inexpensive.
5. Mesh Nebulisers
- Makes use of a membrane that vibrates at a frequency to convert liquid to aerosol medication.
- Small in size and the fastest medicine dispenser.
- Powered via batteries and makes no sound.
- Much more expensive than the others.
- Should be handled with care and frequently cleaned.
Preparing the Nebuliser for a Child’s Breathing Treatment
Before touching any part of the nebuliser, ensure that your hands are washed properly and completely clean. This avoids any external organisms from entering the nebuliser.
- Choose a comfortable spot with a table or a hard surface.
- Remember to clean the air filter of the nebuliser before use. If it is dirty, wash it with cold water and let it dry.
- Plug the machine in the supply socket. Bring the medication ampule and place it in the medicine container of the nebuliser. If your doctor has advised you to mix a few medicines together, use a dropper or a syringe to measure the right quantity of each medicine and then mix them together.
- In some cases, adding saline water to the medication might be required to create a good aerosol. Do not create saline water at home. Always purchase sterile saline from a pharmacy and use it with the medication.
- Place the container and connect it to the machine via the tube.
- Make sure the facial mask is clean and connect it to the top part of the nebuliser.
Advantages and Disadvantages of Nebuliser Treatment
Let’s read below about the advantages and disadvantages of nebuliser treatment.
Advantages
- Nebulisation is an effective method to deliver aerosolised medications.
- It features delivery routes, like pacifiers or masks ideal for infants.
- Nebulisers are available as a portable option too that are easy to travel with.
Disadvantage
- Nebulisers can spread contaminated mist if not properly cleaned between uses.
- Nebuliser takes longer than an inhaler and may require replacement.
- Its use can result in some side effects, depending on the medication used.
Tips for Helping Your Kid Use a Nebuliser
- Establish a fixed routine for using the nebuliser, so that the kid gets acquainted with it.
- Make nebulisation a fun-filled activity, by turning it into a game or telling your kid a story during the process.
- To make your child more comfortable with the machine, you may stick pictures of their favourite cartoons on it.
- When using it on a baby, if he keeps moving constantly, let him sleep. Then, use the nebuliser on the baby, gently, while he is in deep sleep.
- Most kids are afraid of the mask and think they won’t be able to breathe in it. Show them examples. Try wearing it yourself and show your child that you can easily breathe through it.
- Every time your child successfully finishes a round of nebulisation, hug him or give them a high-five. Make it a mission of sorts, where each round helps defeat the enemy germs inside the body.
Cleaning a Nebuliser
It is important to clean the nebuliser and the facial mask after every round, even if there is a subsequent round to be done in a few hours.
- Wash the facial mask and container using a few drops of dish soap and warm water.
- Shake off the water and let it dry.
- Carry out full disinfection of the nebuliser. Except for the mask, every other nebuliser part should be immersed in hot water that contains a few drops of vinegar. Let the parts soak for about 60 minutes.
- Rinse them well and let them dry completely.
- Before putting the nebuliser away, make sure there are no water droplets remaining anywhere.
Side Effects of Nebulisation on Children
Some usual and normal side effects are:
- A dry throat or weird taste in the mouth
- The medicine’s taste can cause a feeling of nausea or heartburn
- In case of strong medication, certain cases might emerge where a kid has a bleeding nose, stomach ache or dizziness
When Should You Call the Doctor?
- The breathing problem aggravates after nebulisation
- The chest tightens or there are rashes and hives on the body
- Your child has a strong headache or starts shivering
- The treatment isn’t having any visible effect at all
FAQ’s
1. Is Nebulisation Only for Children Suffering from Asthma?
No, many other diseases can also be treated via nebulisation. Nebulisation can also be administered using a simple saline solution, for children having a cough.
2. Can I Use Nebuliser at Home?
Nebulisers can easily be used at home. However, no medication apart from sterile saline solutions should be administered without the doctor’s recommendation.
3. Are Inhaler and Nebuliser The Same?
An inhaler is not powered by electricity and is usually handheld to administer asthma-related medication. Nebulisers are used for a variety of purposes, including asthma.
4. Can a Nebuliser Be Used for Respiratory Illnesses As Well?
Yes, as long as your doctor has advised the medicine, the dosage, and the frequency of use.
5. Will My Kid Need to Take Deep Breaths During Nebulisation?
Not at all. Normal breaths are fine.
6. Does Nebulisation Cause Addiction?
There is no addiction since the only difference is the medium of delivering the medication.
7. Does Nebuliser Medicine Use High Dosage of Medicines?
On the contrary, the dosage is less than that present in tablets or syrups.
8. How Can I Choose Home Nebuliser?
Choose a nebuliser that is cost-effective, easy to clean and handle, from a well-known brand, and versatile in usage.
9. Is It Ok to Use Nebuliser for Stuffy Nose?
Depending on the medication to be used a children’s nebuliser can be used for severe cases of a stuffy nose or nasal congestion.
Make sure to conduct your paediatrician if your child has respiratory complaints for a proper diagnosis and treatment. The process of nebulisation for infants can be quite scary at first and babies themselves could be terrified by it. The right environment and the right support can help your child get used to the nebulisation process and get relief from the disease quickly and easily.
References/Resources:
1. How to Use a Nebulizer for a Baby; cchwyo.org; https://www.cchwyo.org/news/2022/august/how-to-use-a-nebulizer-for-a-baby/
2. Home Nebulizer; my.clevelandclinic.org; https://my.clevelandclinic.org/health/drugs/4254-home-nebulizer
3. Side effects of nebulised medication; mylungsmylife.org; https://mylungsmylife.org/topics/group-1/nebulisers/side-effects/
4. Inhaler or Nebulizer: Which One Should My Child Use?; hopkinsallchildrens.org; https://www.hopkinsallchildrens.org/Patients-Families/Health-Library/HealthDocNew/Inhaler-or-Nebulizer-Which-One-Should-My-Child-Us
5. Your Child’s Asthma: Nebulizer Treatments; urmc.rochester.edu; https://www.urmc.rochester.edu/encyclopedia/content.aspx?contenttypeid=90&contentid=P01687
Also Read:
Sinusitis in Kids
Bronchitis in Children
Home Remedies for Runny Nose in Babies and Children
Was This Article Helpful?
Parenting is a huge responsibility, for you as a caregiver, but also for us as a parenting content platform. We understand that and take our responsibility of creating credible content seriously. FirstCry Parenting articles are written and published only after extensive research using factually sound references to deliver quality content that is accurate, validated by experts, and completely reliable. To understand how we go about creating content that is credible, read our editorial policy here.



















.svg)