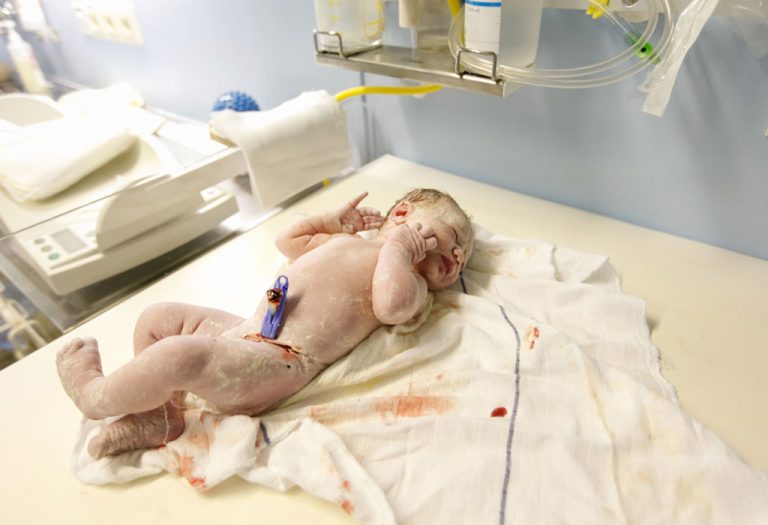
Macrosomia (Big Baby): A Labour complication

Macrosomia is a condition wherein the baby is larger or heavier than a full-term baby. This condition is commonly observed in babies of mothers who are obese or diabetic, and it may lead to certain problems during delivery as the baby may be too large to pass through the birth canal.
What Is Macrosomia (Big Baby)?
The term ‘Macrosomia’ is adapted from the Greek language and literally means ‘macro – large or big’ and ‘somia’ meaning ‘body’ and is usually used to describe a newborn with excessive birth weight. (The average weight of a healthy newborn is about 7 pounds). Macrosomia is also known as the ‘big baby syndrome’.
Foetal macrosomia in pregnancy is defined as the condition where the birth weight of a baby is more than 4000-4500g or 8-9 lbs or more than 90% for gestational age. Women pregnant with a big baby are likely to have a difficult labour. The risk of complications significantly increases when the birth weight is greater than 9 pounds, 15 ounces (4,500 grams).
Various attempts to make a prenatal (before birth) diagnosis of this condition have largely been inaccurate. However, your obstetrician may check for macrosomia if your abdominal measurements or ultrasound indicate that the baby is heavy compared to their gestational age (weeks or months of pregnancy). However, it should be noted that an ultrasound is not accurate during the later stages of pregnancy.
What Can Be the Causes of Macrosomia?
Although most of the foetal macrosomia in pregnancy remain unexplained, various causative factors that may be the reason for having a big baby have been identified. These include:
- Genetics: Parents’ height and weight have an impact on the baby’s birth weight.
- Ethnicity: Hispanic women are more likely to have a large baby as compared to Asian women.
- Duration of Gestation (Pregnancy): It is more common in pregnancies which have crossed the expected date of delivery (E.D.D) by 1-2 weeks or more.
- Presence of Gestational Diabetes or a Known Case of Diabetes Mellitus: A diagnosis of Diabetes Mellitus before or during pregnancy is an alarming risk factor for foetal macrosomia. Uncontrolled diabetes may be linked to higher frequencies of this condition.
- Maternal Age: Women over the age of 35 years are more likely to get pregnant with a big baby.
- Male Child: Male foetuses commonly weigh more than their female counterparts. Most babies above 4500g are usually males.
- Pre-Pregnancy Weight: Excessive obesity or a high BMI before pregnancy.
- Pregnancy Weight Gain: Excessive weight gain during pregnancy.
- Family History: History of a previous macrosomia baby increases the risk by multiple folds.
What Are the Symptoms of Macrosomia?
While there are no specific symptoms of macrosomia, the following are the signs of a big baby during pregnancy:
- Excessive Fundal Height: Foetal macrosomia is usually suspected when your routine antenatal (pre-delivery) visits to a doctor are suggestive of excessive fundal height (maximum distance from the pubic bone to the top of the uterus in the abdomen). It is generally termed as being large for gestational age in the medical language.
- High Weight Gain: Excessive body weight during later pregnancy might be an indirect symptom of having a macrosomia baby.
- Polyhydramnios: Excessive amniotic fluid, which surrounds the uterus and acts as a shock absorber may be associated with this condition. This can be detected by ultrasonography. According to some investigators, polyhydramnios is said to be a result of excessive urine output by a large baby.
Complications
Macrosomia can cause issues for both the mother and the baby. Here is a quick overview of the complications both the mother and the baby may face.
Complications for a Mom-to-be
The major maternal complications of foetal macrosomia occur because of birth injuries and traumatic deliveries.
- Difficult Labour: A baby that is larger than usual may get obstructed in the birth canal during normal labour. This may require assisted deliveries with the help of forceps or vacuum devices.
- Genital Tract Injuries and Lacerations: The excessive force required to deliver a large foetus may injure the vaginal tissues and the perianal muscles (muscles that hold the integrity of the anal canal).
- Excessive Bleeding: Antepartum (birth time) or postpartum (after delivery) bleeding may occur in case of complicated labour due to foetal macrosomia. Here, the birth canal is larger than normal to accommodate the oversized foetus.
- Uterine Rupture: Although rare, a previously operated uterus of a woman, either because of a previous C-section or any other uterine repair procedure may be at higher risk of rupture at the suture site. This is because a macrosomic foetus exerts more strain on the uterine walls.
- Higher Risk Of Foetal Macrosomia In Future Pregnancies: The risk of foetal macrosomia successively increases in probability with each macrosomic delivery.
Complications in Babies
- Birth Time Injuries: In cases of obstructed labour due to foetal macrosomia, babies delivered normally with or without assisted techniques may sustain bodily damage. This includes shoulder dystocia, a mechanical complication wherein due to disproportion the shoulders are not delivered after the head of the baby. It results in the shoulders getting lodged within the mother’s pelvic bone. Neurological complications may also occur due to trauma to the baby’s head during delivery.
- Hypoglycemia at Birth: A baby may be born with excessive birth weight and will be more likely to have lower than normal blood sugar levels at birth. This may be detrimental if not diagnosed instantly and may trigger neonatal seizures. This condition may happen especially if the mother is diabetic.
- Childhood Obesity: Macrosomic babies are prone to obesity in their childhood. The risk is directly proportional to birth weight.
- Metabolic Complications: Babies with excessive birth weight have a higher likelihood of acquiring metabolic syndrome. This is a triad of excessive blood pressure, elevated blood sugars, and abnormal body fat or deranged cholesterol profiles. It is directly associated with a higher risk of future cardiovascular and cerebrovascular diseases in adulthood.
Factors Influencing the Risk of Macrosomia in Women
- Obesity: Obesity may significantly affect pregnancy outcomes, including the incidence of foetal macrosomia in many direct and indirect ways. Body Mass Index (BMI) is measured as weight in kgs/height in meters square. Obesity is described as a BMI of more than 30, while a BMI of more than 25 is considered overweight and a harbinger of obesity. Obese women are more likely to have diabetes mellitus and gestational diabetes, both, in turn, are other direct etiological factors for foetal macrosomia.
- Diabetes Mellitus Or Gestational Diabetes: Women with existing diabetes or that detected during pregnancy are at a higher risk of having a large baby. Blood sugar levels also affect foetal outcomes.
Diagnosis for Big Baby
- Laboratory Method: A glucose tolerance test (GTT) done around 24-28 weeks of gestation can be a good method to rule out possibilities of gestational diabetes. An impaired fasting GTT may suggest further workup and evaluation for Gestational Diabetes Mellitus (GDM) and subsequently for foetal macrosomia.
- Screening Method: Clinical examination including regular abdominal measurements and fundal height may give an idea of the possibility for foetal macrosomia. Specifically, abdominal circumference measuring more than 35cms before 2 weeks of delivery is associated with macrosomic delivery.
- Imaging Method: Macrosomia Ultrasound (USG) of the abdomen can estimate the foetal dimensions from time to time and help correlate them to the gestational age of the foetus.
Treatment for Macrosomia
Treatment of foetal macrosomia includes an integrated approach. Although definitive treatments are subjective for each case, the following is a common protocol advised for foetal macrosomia management.
- Diet: Overweight and diabetic mothers should adhere to balanced and healthy diets. If you’re overweight, get in touch with a dietician, and get a diet plan created for you.
- Medical Obstetric Care: Although induction of labour in cases of foetal macrosomia is a subject of debate, pregnancies more than 39 weeks may be offered induction in a subjective and supervised view to prevent complications.
- Surgical Care: Vaginal assisted deliveries with either forceps or vacuum-assisted devices may be applied for obstructed normal deliveries.
Caesarean section (c section for big baby) may be chosen as an elective or emergency procedure based on the screening results.
Will Macrosomia Affect My Delivery?
Macrosomia in a few cases may result in traumatic deliveries, including vaginal and perineal injuries. There are chances of excessive haemorrhage and rare instances of uterine rupture. It may necessitate assisted vaginal or caesarean section delivery. Macrosomia also increases the chances of having foetal macrosomia in successive future pregnancies.
Will Macrosomia Affect My Baby’s Health?
Macrosomia may affect the baby during delivery, including birth time hypoglycemia, shoulder dystocia, and neurological damage. It may also predispose the baby to have obesity, diabetes mellitus, cardiovascular and stroke-like diseases in the future.
Can Macrosomia Be Prevented And Managed?
Yes, with timely medical consultations, regular antenatal follow-ups and scanning, macrosomia can be prevented. Also, efficient weight control with dietary measures, regular exercise, and adequately controlled sugars with medications can help prevent macrosomia.
How to Lower the Chances of Having a Big Baby
Early diagnosis of gestational diabetes and proper management can lower the chances of foetal macrosomia.
Macrosomia is a labour complication for the mother and disease predisposing for the baby in future. However, it can be well estimated during pregnancy with frequent and timely scans. It can also be effectively prevented by changing lifestyle measures and managed or treated with assisted delivery techniques.
Also Read: Foetal Growth Chart Week By Week – Length & Weight
Was This Article Helpful?
Parenting is a huge responsibility, for you as a caregiver, but also for us as a parenting content platform. We understand that and take our responsibility of creating credible content seriously. FirstCry Parenting articles are written and published only after extensive research using factually sound references to deliver quality content that is accurate, validated by experts, and completely reliable. To understand how we go about creating content that is credible, read our editorial policy here.