How Does Having Gestational Diabetes Affect Your Delivery Options?
Pregnancy is certainly one long roller coaster ride. Every to-be mother goes through her share of ups and downs during her gestation period. The upside is the joy, the pampering, the gifts, and pure bliss on some days. The downside could be anything from feeling fatigued to gestational diabetes. Many pregnant ladies are worried about complications and risks of having gestational diabetes (GD). We discuss the implications of having gestational diabetes and what care is required during pregnancy.
Gestational Diabetes Mellitus is an intolerance, of any degree, to glucose where the onset is recognised during pregnancy. Data suggests that around 7% of pregnancies are sure to have GDM. Cases differ from one individual to another where some are dependent on insulin, while others are treated through a modified diet. Gestational diabetes is usually detected through screening at the first prenatal visit. Screening is repeated after 24 weeks to make sure that gestational diabetes is not present. A fasting glucose test with levels greater than 126 mg/dl or a random glucose test with levels higher than 200 mg/dl indicates diabetes. Women who present as high-risk cases are usually diagnosed through a glucose tolerance test (GTT) or a glucose challenge test (GCT).
Having gestational diabetes does not impair your chances of having a healthy baby. You simply have to manage your blood sugars well with help from your doctor and your family. Let us understand what risks are involved and how you can overcome them.
Can Gestational Diabetes Affect Your Birth Options?
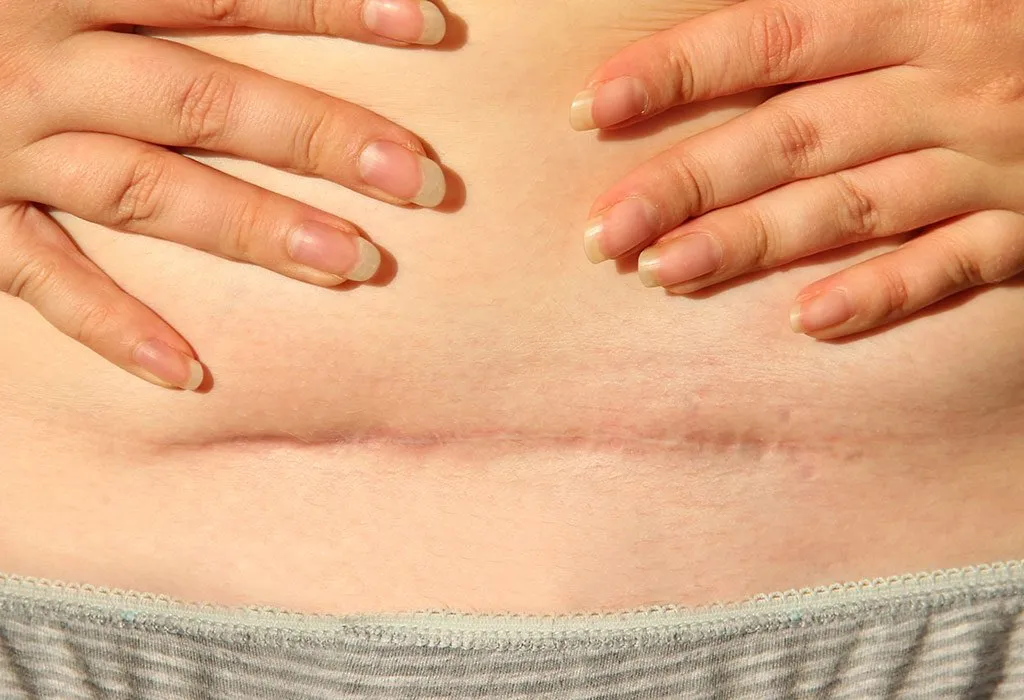
The high blood sugar levels during gestational diabetes can make your baby grow a lot bigger than usual. Giving birth to a bigger baby can cause excessive blood loss and tears in the perineum. An alternative is a C-section birth, but a surgery has its own risks like infection, excessive bleeding, risk of a heart attack, and problems with future pregnancies.
Gestational diabetes increases your risk of requiring a C-Section. However, if your sugar levels are under control, you can have a vaginal delivery. The size of your baby is the key to deciding whether you will be able to have a safe vaginal delivery.
Is Vaginal Birth Possible When You Have Diabetes While Pregnant?
Gestational diabetes does not mean you cannot have a vaginal delivery. It all depends on how controlled your blood sugar levels are. The crucial thing you should remember is that you do not cross your due date. Your doctor will want to induce labour by the 40th week if there are no signs of natural labour by then. If you require medication to keep your gestational diabetes under control, then your doctor would want to induce your delivery after the 38th week. The reason for concern with high blood sugar is that the pregnant woman is at a higher risk of developing preeclampsia.
Another risk of high blood sugars is macrosomia, or having a big baby whose birth weight is more than 4.5 kilograms. There are certain complications that may arise because of a large sized baby.
- A big baby could lead to a larger tear in the perineum
- It could cause more loss of blood.
- There is a chance of the coccyx (the tail bone) being damaged during delivery.
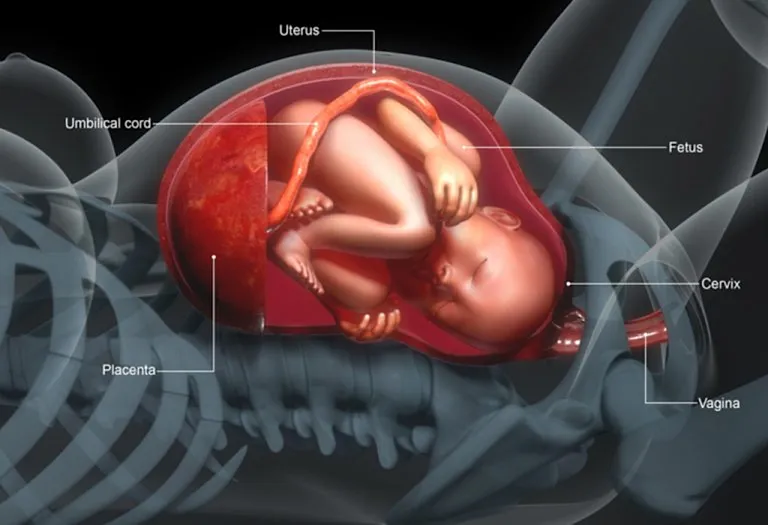
- One in 13 babies over the weight of 45kgs have shoulder dystocia. This is when the baby’s shoulder is stuck behind the pelvic bones. High sugars cause the baby to be bigger around the chest and shoulders.
- The dystocia, in turn, could squash the umbilical cord, cutting off the baby’s oxygen supply before delivery.
Getting into the right delivery position can help your baby, and there are chances you could successfully have a vaginal delivery. It is important to consult your physician before you make a decision about gestational diabetes and normal delivery.
Does Gestational Diabetes Increase the Risk of Preterm Labour?
There are chances of delivering early with gestational diabetes. The placental hormones that are released during pregnancy make the mother resistant to insulin. High blood sugars make the baby gain weight faster. A bigger baby surrounded by excess fluid could make the body think it is further along gestation that it actually is. This can lead to pre-term delivery. Most complications that are linked to gestational diabetes have to do with poor control over blood sugar. Gestational diabetes and premature birth can be checked by taking the right precautions through portion control, exercise, and meal planning. This makes diet and exercises a crucial component in fighting gestational diabetes.
One major reason to induce preterm labour is to avoid the risk of stillbirth. Due to very high blood sugar, a pregnant mother may be affected by high blood pressure, microvascular conditions, or poor blood circulation. This causes the foetus to develop very slowly sometimes, and can lead to stillbirth. Although the exact cause is not known, stillbirth is higher in women with poor blood glucose control.
Does Gestational Diabetes Mean You Need Extra Monitoring During Labour?
Additional monitoring during labour is crucial for pregnant women who have gestational diabetes. The blood glucose requires to be checked every hour to make sure that it stays in the safe range during delivery. If the glucose levels increase, then additional insulin should be administered as drips. Additional insulin will mostly be necessary if you have been taking insulin injections to keep blood sugar under control. Assisted delivery may also be required if the mother becomes fatigued or the baby is distressed during the delivery. Instruments like forceps delivery or suction caps (ventouse) may be required to aid the baby during delivery. Assisted deliveries may leave small marks or bumps on the baby’s head that will fade over the next few weeks.
Several pregnancies with gestational diabetes have needed to be induced into labour or have a caesarean birth due to the need of the hour. Labour may take up to 24 hours to commence after an induction. Induction is generally done using vaginal gel, drips to the arm, or a pessary. The contractions are different to what is felt in a natural delivery. Contractions will be much closer together and certainly more powerful. Baby’s heartbeat will be constantly monitored during this time. If you have not made enough progress after induction and if your baby is coping well, you will be induced a second time. If this does not bring in the desired results and labour isn’t progressing, then a caesarean will be recommended.
A caesarean or a c-section is a surgery where your baby is brought out through a tiny incision made in your lower abdomen. It is termed as an emergency c-section when it is unplanned and is required because induced labour has not progressed as planned.
The upside to being pregnant, with or without diabetes, is delivering a beautiful and perfect baby. Gestational diabetes is a small snag in an otherwise lovely adventure, and it can be managed through control and caution. Your delivery may have none of the complications associated with gestational diabetes, or you might have a few unexpected changes. Ultimately, it is more important to have delivered a healthy baby than fret over how the delivery happened. Reading up and being prepared always helps mothers to prepare for what is imminent mentally. So, read up, be ready, and have yourself the most gorgeous baby ever!
Also Read:
Tips for Easy Labor and Delivery
Does Eating Pineapple Help to Induce Labour
Can Acupuncture Help in Inducing Your Labour
Was This Article Helpful?
Parenting is a huge responsibility, for you as a caregiver, but also for us as a parenting content platform. We understand that and take our responsibility of creating credible content seriously. FirstCry Parenting articles are written and published only after extensive research using factually sound references to deliver quality content that is accurate, validated by experts, and completely reliable. To understand how we go about creating content that is credible, read our editorial policy here.