Epilepsy in Pregnancy: Symptoms, Complications & Treatment
- What is Epilepsy?
- Does Epilepsy Make it More Difficult to Conceive?
- Symptoms of Epilepsy in Pregnancy
- Does Epilepsy Change During Pregnancy?
- Diagnosis
- Complications
- Treatment
- Medication for Epilepsy
- Epilepsy and Labour
- FAQs
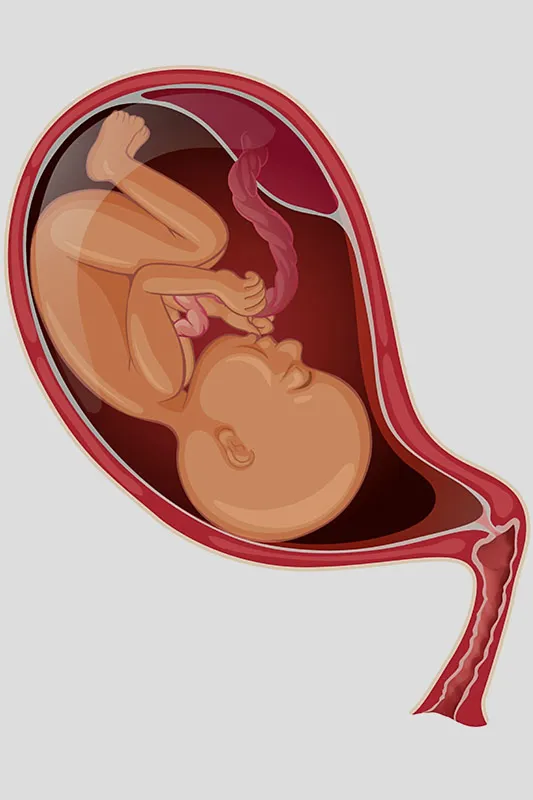
Being pregnant is not easy, and if a woman has epilepsy during pregnancy, the nine months of pregnancy could be even more difficult for her. Epilepsy is a disorder of the nervous system, and is also called a seizure disorder. A majority of epilepsy-related seizures aren’t dangerous by themselves. However, the timing of an epileptic attack can be dangerous as people may end up injuring themselves or people around them. Having an epileptic attack during pregnancy, on the other hand, can cause complications such as slowing of the foetal heart rate or a miscarriage. Read on to know more about epilepsy during pregnancy, and how it affects the health of a pregnant woman and her unborn child.
What is Epilepsy?
Epilepsy can be defined as a disorder of the nervous system, in which a person experiences recurrent seizures. These seizures could be very mild and hardly show any symptoms or they could be last for long and cause shaking of the muscles.
Does Epilepsy Make it More Difficult to Conceive?
In earlier years, women with epilepsy were discouraged from having children. However, this has changed in recent times with the availability of better prenatal care. Around 90% of women with epilepsy have fewer complications and deliver healthy babies.
Epilepsy and pregnancy can lead to problems like:
- Polycystic ovarian syndrome (PCOS): Women with epilepsy are more likely to have PCOS, a primary cause of infertility.
- Anovulatory cycles: Women with epilepsy are more likely to have menstrual cycles where an egg may not be produced, reducing the chances of pregnancy.
- Anti-seizure drugs: These drugs, which are administered to women with epilepsy may interfere with the hormone levels in the ovary, leading to infertility.
- Irregular menstrual cycles: This is a common occurrence among women who are pregnant, and it may affect their chances of conceiving.
- Hormonal abnormalities: Women with epilepsy are likely to face hormonal abnormalities which make it difficult to sustain a pregnancy.
Despite these complications and risks, a majority of women who have epilepsy can successfully carry a baby to term.
Symptoms of Epilepsy in Pregnancy
The symptoms of epileptic behaviour depend on the type of epilepsy that a woman has. These symptoms of epilepsy are similar to those of the symptoms experienced during pregnancy. Some of the common symptoms are listed below.
- In case the pregnant woman suffers from partial epilepsy, then she may experience dizziness and lose consciousness during the seizures.
- Absent-mindedness, the woman may stare blankly for 5 to 20 seconds which may go up to 5 minutes in severe cases.
- For some women, there may be a loss of memory also.
- Mood swings are also a symptom of epilepsy in pregnancy.
- The pregnant woman may experience nausea, vomiting, anaemia and increased vaginal bleeding.
- If the seizure activity increases in expectant mothers, then there may be several bodily changes.
- Similar to the increase in seizure activity, there could be a decrease in progesterone levels.
- While epileptic seizures remain the same for most women, they may change in some cases. This change is essentially when the seizures are not monitored properly.
Does Epilepsy Change During Pregnancy?
While it is believed that mostly there is no change in epilepsy during pregnancy, in some cases the frequency of seizures may increase. The reason for this increase is due to the medication prescribed for controlling the seizures. They are known as anticonvulsants. These tend to start working differently during pregnancy. Hence, your doctor may need to change the medication during pregnancy.
Diagnosis
The diagnosis of epilepsy and seizures should be done by a neurologist. Women having epilepsy must keep themselves abreast of the different types of epilepsy so that they are aware of the risks involved such as hypertension and premature labour.
In case a pregnant woman suffers from epileptic seizure during the later part of the pregnancy, it may not be attributed entirely to epilepsy. She should be treated on an immediate basis keeping in view eclampsia management till a complete diagnosis is made by a neurologist.
Other conditions like cardiac, metabolic, intracranial and neuropsychiatric conditions should be kept in view while the diagnosis is being done.
Complications
Epilepsy and its medications affect both the mother and baby during pregnancy. While most women have a relatively normal pregnancy, there may be some risks associated with epilepsy during pregnancy. These risks include:
-
Hypertension
This can have an impact on the blood flow to the placenta leading to premature birth.
-
Trauma
In some cases, seizures are associated with loss of consciousness and violent movement leading to trauma or fall which may lead to premature labour.
-
Neural Tube Defects
These include issues with the nervous system such as the brain, spinal cord, and nerves.
-
Excessive Bleeding
Severe bleeding in the baby because of lower levels of vitamin K.
-
Addiction
Babies may show withdrawal symptoms after birth because the anti-epileptics are stopped.
Treatment
The most important thing to do during pregnancy to make it a success is to monitor and manage epilepsy; this includes pre-natal and post-natal care.
A woman with epilepsy should visit her doctor more often during pregnancy. The medications prescribed to prevent and control seizures should be carefully monitored for any complications. They should be prescribed in small doses.
As per statistics, 2 to 3% develop malformations in the foetus (cleft lip and cleft palate) due to the dosage of the anti-epileptic medicines. Hence the medication should be prescribed after a complete evaluation.
Apart from medication, one can make modifications to their lifestyle such as consuming a healthy diet, abstaining from drugs and getting adequate sleep.
Medication for Epilepsy
Medication with the fewest side effects should be used to treat epilepsy during pregnancy. Valproic acid and lamotrigine are relatively safe epilepsy medication in pregnancy though valproate if used during the initial 28 days of pregnancy, has a 1 to 2% risk of neural tube defects.
Epilepsy and Labour
As a woman reaches the last stage of her pregnancy and labour is near, she is likely to have a lot of questions and concerns regarding the delivery and how the seizures may impact the same.
Mostly women who have epilepsy have a vaginal delivery without any risk. In case there is a risk of seizure during delivery, or within the next 24 hours, the childbirth needs to happen in a separate maternity unit under the guidance of a consultant. This is done to ensure that proper care and facilities are available during the delivery and later. This, however, depends on your last seizure and the medications that you are currently taking.
There are a few options that can be used for pain-free labour:
- Doing breathing exercises could be helpful for pain relief, but they should be done in moderation as they could trigger a seizure.
- Women with epilepsy could be given epidurals.
- Pethidine which is a pain relief drug could also trigger seizures so it should be taken in consultation with the doctor. Diamorphine may be used instead.
FAQs
1. Will I Need More Folic Acid Than Other Pregnant Women Do?
While it is essential to take appropriate medication for epilepsy, it is also important to take doses of folic acid. Prior to conception, folic acid should be taken at a dosage of 4 to 5 mg every day. This is higher than other prenatal vitamins taken during pregnancy. Usually, about 50% of pregnancies are unplanned, and the woman only comes to know about it after about 4 weeks. Hence, a folic acid dosage is recommended to all women having epilepsy who fall in the childbearing age. You should consult your doctor before you start the folic acid dosage.
2. Can I Breastfeed if I am Epileptic?
Yes, a woman with epilepsy can breastfeed the baby while being on anti-seizure medication. This medication is also secreted through in the breast milk and the baby is exposed to some amount. However, the benefits of breastfeeding outweigh the potential risks attached to the medication.
3. When Should I Call a Doctor?
Mentioned below are the situations when a woman with epilepsy should call the doctor immediately:
- If the woman having seizures stops breathing for more than 30 seconds.
- If the seizure lasts for more than 3 minutes, then it is a serious, life-threatening situation called epilepticus.
- If the woman has more than one seizure in a duration of 24 hours.
- If the woman having the seizure is not responding within an hour after the seizure has occurred and has any of the below-mentioned symptoms:
- Nausea or vomiting
- Confusion or dizziness
- If the woman is in a state of reduced consciousness, i.e., neither completely unconscious nor fully conscious.
- If the seizure is followed by a head injury.
- If a diabetic woman has had a seizure, low blood sugar, or high blood sugar.
- If the woman is complaining of a severe headache right after the seizure has occurred.
- If the seizure has signs of a stroke like issues with speaking or understanding, vision loss and having trouble in movement.
Epilepsy is a disorder that can be treated with medication. These medicines may have side effects, hence to make sure that they work effectively, check with your doctor and follow his advice.
Also Read: Migraines During Pregnancy: How to Deal With It?
Was This Article Helpful?
Parenting is a huge responsibility, for you as a caregiver, but also for us as a parenting content platform. We understand that and take our responsibility of creating credible content seriously. FirstCry Parenting articles are written and published only after extensive research using factually sound references to deliver quality content that is accurate, validated by experts, and completely reliable. To understand how we go about creating content that is credible, read our editorial policy here.