Thyroid Problem After Pregnancy

- What is Thyroid?
- How Can Childbirth Affect a Woman’s Thyroid Condition?
- Can Thyroid Medication Affect Milk Supply?
- Can Thyroid Medication Pass into the Breast Milk and Affect a Child?
- How Common is Congenital Hypothyroidism and Hyperthyroidism in Newborns?
The postpartum phase is not easy for all moms. It’s common to experience fatigue and back pain after childbirth, but some women may also develop thryoid, also called postpartum thyroiditis. The risk of developing postpartum thyroid is higher in women who have Type 1 diabetes. In fact, women who have experienced this condition before are forty per cent more likely to develop it again. This article will help you understand the causes, complications and treatment methods to combat postpartum thyroid.
What is Thyroid?
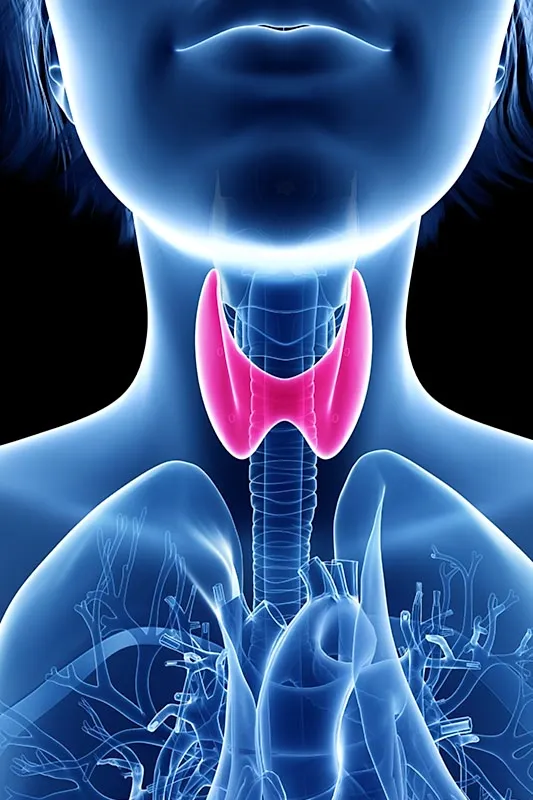
The thyroid is a small butterfly-shaped endocrine gland located in the anterior of the throat. Endocrine glands are those which produce hormones essential for the body, in this case, thyroid hormones, T3 and T4. These hormones are essential in metabolism that is in the cellular production of energy. They are also important in the regulation of body temperature as well as organ functioning.
How Can Childbirth Affect a Woman’s Thyroid Condition?
Thyroid after pregnancy can often be overlooked and can remain undiagnosed for long. This condition can develop and affect in the following ways and each requires different treatments.
1. Hypothyroidism
Hypothyroidism is due to the thyroid gland functioning at low levels, producing lesser thyroid hormones than required. Symptoms include fatigue, weight gain, constipation and body aches. Hypothyroidism can be controlled by administering the synthetic hormone, levothyroxine, which can make up for the lack of thyroid hormones. Levothyroxine has minimal to no side effects and can be taken indefinitely without any long-term complications. Approximately half the women with postpartum hypothyroidism develop a more severe case called Hashimoto’s Thyroiditis, which can be treated by increasing the medication dose.
2. Hyperthyroidism
Hyperthyroidism is caused when the thyroid gland overproduces hormones. It affects less than one per cent of pregnant women. An autoimmune disease known as Graves’ disease is often the cause of hyperthyroidism. During pregnancy, this condition can cause preterm labour, hypertension, placental abruptions, uterine tearing, preeclampsia and so on. Treating hyperthyroidism involves a range of antithyroid medications, such as propylthiouracil and methimazole. The risks associated with these medications are rare but they can sometimes lead to birth defects. In order to avoid this, doctors may recommend a minor surgery known as a thyroidectomy. In this case, the surgical procedure removes part of or the entire thyroid gland in order to avoid the symptoms of hyperthyroidism symptoms.
3. Postpartum Thyroiditis
Postpartum thyroiditis is a rare disease wherein a perfectly functional thyroid gland undergoes inflammation within the first few months after giving birth. It can take a few weeks to several months or even years to subside. This condition is tricky to diagnose as the signs are often confused with postpartum depression and stress that most new mothers go through after childbirth. While most mothers have their thyroid glands back to normal within a year or so after birth, some women might end up having complications for the rest of their lives.
Postpartum thyroiditis occurs in around five to seven per cent of new mothers. Since the immune system attacks the thyroid during this condition, it first causes hyperthyroidism which then leads to hypothyroidism. This results in an increase in thyroid hormone concentrations in the bloodstream, leading to thyrotoxicosis. Its symptoms include stress, irritable behaviour, inability to tolerate heat, raise in appetite, sleeplessness, anxiety, increased or palpitations, body tremors, and so on. In time the hyperthyroidism abates, which is due to a depletion in the levels of the thyroid hormones. After this, the symptoms of hypothyroidism set in. These are tiredness, dry skin, mood problems, reduced appetite, inability to bear cold, and so on. Postpartum thyroiditis hair loss is another common symptom that affects many women.
Since these symptoms match with postpartum depression, also known as the baby blues, this condition is often misdiagnosed. Treatment during the first phase of hyperthyroidism is often not required as the symptoms are tolerable and temporary. If they are unbearable, your doctor will prescribe you beta-blocker drugs which can calm anxiety and reduce heart rate. Hypothyroidism requires hormone replacement therapy with levothyroxine, as already mentioned before.
Can Thyroid Medication Affect Milk Supply?
Thyroid medication—whether synthetic hormones or antithyroid drugs—does not affect the milk supply if given in low does. The medication is prescribed keeping in the mind the breastfeeding status of a new mother. On contrary, the lack of medication can certainly have a negative impact on it. This is because both hypothyroidism and hyperthyroidism can affect the milk supply. In both these conditions, there is an influx of certain hormones like FIL, known as the feedback inhibitor of lactation. This results in the reduction of lactation, which subsequently leads to the reduction or stoppage in the milk supply entirely. A simple treatment technique involves massaging the breasts slowly downwards while moving towards the nipples. This has been known to stimulate the production and release breast milk.
Can Thyroid Medication Pass into the Breast Milk and Affect a Child?
Hypothyroidism medication, levothyroxine, is completely safe, as it is found in breastmilk at negligible levels or not at all. However, hyperthyroid drugs like propylthiouracil and carbimazole require monitoring of the baby’s thyroid functions. This is because it can cause neonatal hypothyroidism in infants. Radioactive iodine treatment is not recommended while breastfeeding a baby.
How Common is Congenital Hypothyroidism and Hyperthyroidism in Newborns?
1. Congenital Hypothyroidism
In most cases, congenital hypothyroidism is due to an underdeveloped thyroid. This condition is extremely rare, occurring in less than one per cent of all babies. Some of the causes include:
- Iodine-deficient Diet: When a new mother does not not include enough iodine in her diet, which is an essential requirement for the foetus’ thyroid gland in the production of the thyroid hormones, a baby may have hypothyroidism. It is common in regions of the world which lack iodine in their diet. Babies born with hypothyroidism usually receive treatment to fix this condition.
- Thyroid Medicines: Sometimes thyroid drugs can cause temporary congenital hypothyroidism, but this kind usually subsides a few days after childbirth.
- Genetic Causes: In rare instances, congenital hypothyroidism can be caused by genetic defects in certain genes. This leads to malfunctions in the synthesis of the thyroid hormones.
The symptoms of congenital hypothyroidism include puffed faces, inflamed tongues, dull appearance, constipation, dry skin and hair, jaundice, fatigue, refusal to eat, delayed fusion of fontanelle, improper weight gain, and so on.
2. Congenital Hyperthyroidism
This disease is uncommon in newborns. It can be caused by maternal Graves’ Disease, in which the thyroid-promoting antibodies enter the placenta and affect the baby’s thyroid gland development. In other cases, the condition can be temporary and is known as transient gestational hyperthyroidism. It’s known to affect around five per cent of babies.
While most mothers recover from post-pregnancy thyroid conditions, around thirty per cent of women tend to experience thyroid problems permanently. This might mean being on medication for long. If you have recovered from postpartum thyroiditis, it is recommended that you go test every three months in the first year followed by yearly testing. It is important to have a support system during this time, especially since the postpartum period comes with a host of potential problems in addition to thyroid diseases. Make sure your family, partner and friends are aware of your condition, so that they can help you whenever you need it.
Also Read: Thyroid during Pregnancy
Was This Article Helpful?
Parenting is a huge responsibility, for you as a caregiver, but also for us as a parenting content platform. We understand that and take our responsibility of creating credible content seriously. FirstCry Parenting articles are written and published only after extensive research using factually sound references to deliver quality content that is accurate, validated by experts, and completely reliable. To understand how we go about creating content that is credible, read our editorial policy here.