Infantile Hemangioma – Causes, Complications and Treatment

Watching their child feel unwell can be devastating and extremely hard to cope with for most parents. Tumours are one of the scariest medical issue and most people instantly associate tumours with cancer. However, there are certain tumours that are non-cancerous and are known as benign. Some of these are known as Hemangioma. It is important to remember that certain types of hemangioma, like capillary hemangioma in newborns, may take over 8 weeks to become diagnosable. Only in about 30% cases are they present at birth.
What is an Infantile Hemangioma?
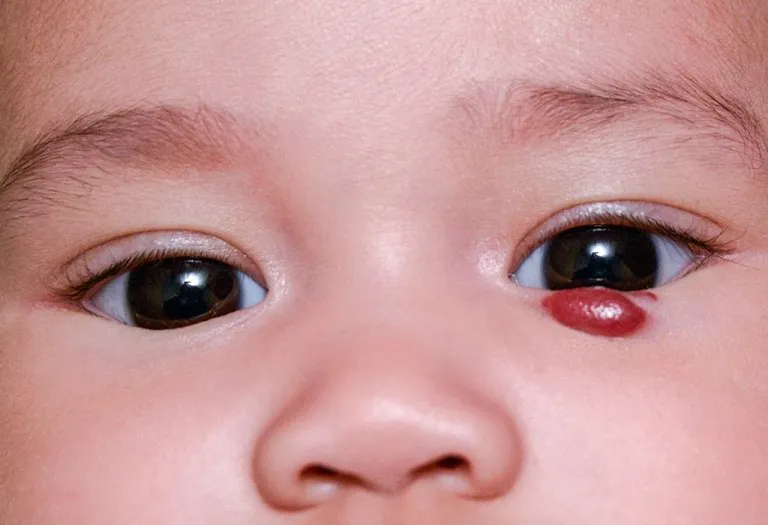
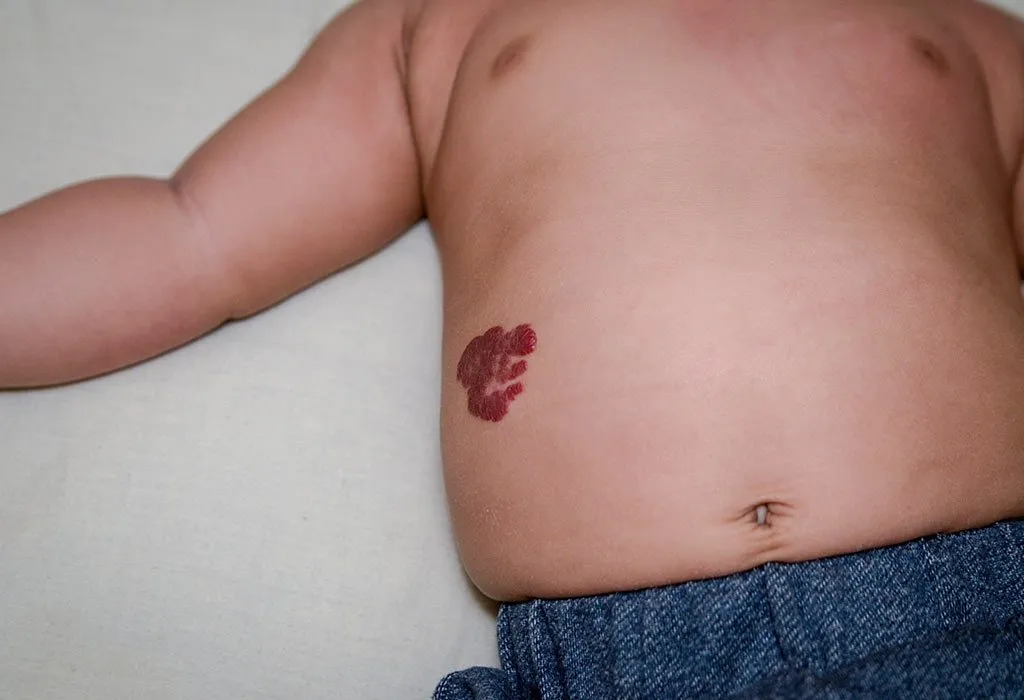
Infantile hemangioma is a benign tumour of the vascular nature and is known to form along the line of blood cells known as endothelial cells. This type of tumour is estimated to be the most common amongst infants and manifest in nearly 5% of all babies. It is assumed that some variants of hemangiomas can be seen at birth and manifest as a strawberry hemangioma birthmark due to the burgundy discolouration of the condition being visible on the skin.
How Does Hemangioma Develop in Babies and Where Does It Occur?
Hemangiomas manifest due to causes yet to be determined by researchers and medical professionals. There is an assumption made on the role of the placenta, but this has no concrete evidence. Doctors consider the following as risk factors.
- Low birth weight
- Premature birth
- Vaginal bleeding early in the pregnancy
These hemangiomas can manifest in numerous parts of the body. Some places are more common than others, but infant hemangiomas on the lip are more common than those on the toes. Here are some of the most common places it occurs:
- Lips
- Forehead
- Forearms
- Fingers
- Chest
- Neck
- Liver
- Colon
- Lungs
- Brain
Hemangiomas develop differently on the skin than they do on internal organs. The ones on the skin are more visible, start from one point and resemble a birthmark before moving upwards and increasing in size.
What Do Infantile Hemangiomas Look Like?
Most hemangiomas can be categorised into three sections.
1. Superficial Hemangiomas
Superficial hemangiomas are the ones located closer to the skin. These appear like birthmarks that are bright red. They can be either flat or a bit bumpy at first and begin protruding upwards. This type of hemangioma can grow rapidly in the first 7-12 weeks. You may also begin seeing the veins beneath or around the hemangioma.
2. Deep Hemangiomas
If the hemangioma develops deeper than the surface level ones and begins to manifest on the nerves, organs or muscles, these are known as deep hemangiomas. Due to its location being much deeper in the body, the red and blue hue is mostly seen only after 6 weeks on the skin, if at all.
3. Mixed Hemangiomas
When an infant is diagnosed with both a superficial and deep hemangioma, then it is called a combined or mixed hemangioma. This type of hemangioma is less common and begins to manifest in both the skin and a deeper layer of the body.
What Causes Hemangioma in Babies?
When a part of your baby’s body begins to collect blood cells at an abnormal rate around one centre to form a tumour, it can be defined as a hemangioma. The exact reason or cause for these blood cells to collect at an abnormal rate is unknown, but multiple causes are being researched.
Signs and Symptoms of Hemangioma in a Newborn
There can be numerous signs and symptoms to indicate your little one has a form of hemangioma. Here are a few signs and symptoms:
Superficial hemangiomas can be visible on patches of skin and have bright burgundy or red colouration, this can resemble a birthmark but will grow at a rapid rate in the first 4- 8 weeks.
Deep hemangiomas can have the following symptoms:
- Abdominal pain and discomfort
- Nausea
- Failure to feed your child due to loss of appetite
- Excessive vomiting
- An inflated abdomen
- Extreme and unexplainable weight loss
Most of the symptoms above can indicate hemangiomas on an internal organ but they are also generally indicative of various other conditions. To get a complete diagnosis, please visit your health care advisor.
Age-By-Age Hemangioma Growth
| Approximate Age | Phase | Stage |
| 4 to 8 months | Growth | The Hemangioma will grow rapidly with puffiness and a bright red colour |
| 5 to 12 months | Resting | The skin will become shiny with no changes in size |
| 1-4 years | Shrinking | The lesion shrinks and the colour changes to purple and grey, and might disappear entirely |
Complications Associated With Hemangioma in Infants
This condition, although it is not cancerous, can have major complications and concerns. Here are a few hemangioma baby challenges that you may need to consider.
1. Interference With Organ Function
A deep hemangioma can manifest on the organs, which can hinder the ability of the organ to function in a manner that is healthy and safe. This can also compromise the condition or health of the organ, forcing it to fail. These conditions are not guaranteed but the concern is large enough to have your doctor monitor your baby closely enough. These blood vessel tumours can also lead to an impaired blood circulatory system that can harm the health of the organ and the functions of other aspects of the body like muscles and ligaments. They may also compress the airway and cause respiratory issues.
2. Ulceration
A hemangioma, while not cancerous, can lead to painful ulcers. This, and the stifled blood circulation, can harm your baby’s overall health in a negative way that, if left untreated, may even become dangerous. It is recommended that you speak to your doctor about ulcerations due to hemangioma and understand how to manage and combat it.
3. Bleeding
As with most conditions that directly involve blood cells, there is a risk of heavy blood loss or consistent bleeding. Hemangiomas can also impair the body’s ability to clot blood in rare cases. This is not a common thing but it does happen and we recommend you consult your healthcare specialist for more accurate information about your baby’s case specifically.
How is Hemangioma Diagnosed?
They are usually superficial and the diagnosis is pretty much apparent to the doctors. However, in most cases, doctors may correlate your baby’s medical and family history to identify the source of the anomaly, which in this case would be a hemangioma. If there is still a doubt, then the doctor could recommend a non-invasive diagnostic tool like ultrasonography, to check for underlying issues. An MRI or CT scan may be ordered to look for some rare neurocutaneous disorders, that may be associated with these hemangiomas.
Infantile Hemangioma Treatment
Here are a few methods used to treat infantile hemangioma in infants.
1. Corticosteroid Medication
The treatment through drug therapy is often considered the first step. A corticosteroid is, in essence, a steroid used to combat blood clots. As with most steroids, it is recommended that your child does not get immunisations that affect the liver or medication for the liver. A common drug for infantile hemangioma is propranolol.
2. Beta-Blockers
Beta-blockers are used as a topical treatment for small and superficial occurrences of hemangioma. The beta-blockers can be used several times in the day for babies between the ages of 6 to 12 months. This treatment is also used for small ulcerated hemangiomas.
3. Laser Treatment
Laser treatment for hemangioma in infants is a common treatment as it not just removes the hemangioma, but also removes the redness and promotes quick healing. Pulsed dye lasers are usually the treatment of choice.
4. Medicated Gel
Medicated gels that contain becaplermin is used to treat ulcers on the surface of the skin hemangioma. As such, this gel does not have any effect on the hemangioma itself. This gel has does carry the risk of cancer and must be used sparingly only under your doctor’s advice.
5. Surgery
In the case of the hemangioma occurring in a sensitive area such as the eye, your doctor might recommend surgery to remove the same. This line of treatment is also recommended for large hemangioma.
Additional Facts About Hemangiomas
- Under a microscope, hemangiomas look very similar to a tangle of blood vessels. In fact, the cells that make up hemangiomas are most similar to those that line blood vessels.
- Technically, a hemangioma is a type of tumour. Unlike a cancerous tumour, a hemangioma will stop growing and disappear with time.
- Hemangiomas do not occur due to any actions taken or not taken during pregnancy.
- Though hemangiomas disappear in due time, you also have other treatment options to remove them entirely.
- As the cells in the hemangioma multiply, the lesion will swell rather than spreading.
FAQ’s
Here are some answers to frequently asked questions about Infantile Hemangioma
1. Do Hemangiomas Hurt the Baby?
Hemangiomas hurt only when there is ulceration on the hemangioma’s surface. However, ulceration begins even before you can see them. Thus, if your baby seems to be in pain, then you must bring it to your paediatrician’s attention.
2. Can a Hemangioma Leave a Scar on My Baby?
Scarring due to a hemangioma is entirely up to the nature of the hemangioma. The location and size are the primary factors for a case of scarring, especially if the hemangioma is in a location where the skin does not stretch as easily such as the nose, lips, forehead, and ears. If the hemangioma ulcerates, then the chances of scarring increases.
3. Can My Baby Have More Than One Hemangioma?
About 20% of babies with this condition have multiple hemangiomas.
4. Are My Future Kids at Risk?
Some studies do suggest that hemangiomas run in families though this has not been proved. Family history is noted in about 12% of the cases. Hemangiomas rarely are associated with Neurocutaneous syndrome and other underlying conditions like PHACE syndrome, Sturge Webber syndrome, etc. Such syndromes can warrant further checks if required by the doctor.
While hemangiomas are considered tumours, they are not cancerous. There are other risks present but this condition is not necessarily fatal. It is strongly recommended that you consult your primary physician and follow their instructions. Do not self-medicate. Combining holistic medication with traditional medication is not recommended and, if you choose to do so, please consult your doctor before attempting this.
Also Read:
Mongolian Spots in Infants
Port Wine Stain in Babies
Was This Article Helpful?
Parenting is a huge responsibility, for you as a caregiver, but also for us as a parenting content platform. We understand that and take our responsibility of creating credible content seriously. FirstCry Parenting articles are written and published only after extensive research using factually sound references to deliver quality content that is accurate, validated by experts, and completely reliable. To understand how we go about creating content that is credible, read our editorial policy here.
























.svg)